How therapists empower recovery in home stroke rehab
Many people assume that hospital-based therapy is the only effective option after stroke, but home rehabilitation reduces poor outcomes significantly when guided by skilled therapists. The truth is, therapists bring specialized expertise directly into your living space, creating personalized recovery plans that address your unique challenges and environment. This article explores how physical, occupational, and speech therapists transform home settings into powerful rehabilitation spaces, what methods they use to accelerate neurological recovery, and how you can maximize these professional partnerships for better functional outcomes.
Table of Contents
- Key takeaways
- Understanding the role of therapists in home rehabilitation
- How therapists enhance recovery through proven methods
- Assessing and adapting the home environment for effective rehab
- Challenges and tailoring therapy for complex cases in home rehab
- Discover tools to support your home rehabilitation journey
- FAQ
Key Takeaways
| Point | Details |
|---|---|
| Home Based Rehab | Home based rehabilitation reduces poor daily living outcomes when guided by skilled therapists. |
| Therapist Roles | Physical therapists focus on mobility, occupational therapists on daily living skills, and speech therapists on communication and swallowing. |
| Home Environment Adaptation | Therapists assess furniture layout and routines to tailor interventions to the patient and their living space. |
| Neuroplasticity Driven Methods | Therapists use evidence based methods like task specific training, constraint induced movement therapy, and mirror therapy to drive neuroplastic changes. |
| Caregiver Engagement | Caregiver training and involvement boost adherence and support practice in daily life. |
Understanding the role of therapists in home rehabilitation
Therapists bring distinct yet complementary skills to your recovery journey. Physical therapists focus on mobility, occupational therapists on daily living skills, and speech therapists on communication and swallowing challenges. Each professional evaluates your specific impairments and designs interventions that fit your home layout, daily routines, and recovery goals.
Physical therapists work on restoring movement patterns essential for walking, transferring from bed to chair, and maintaining balance. They analyze how your furniture placement, floor surfaces, and room transitions affect mobility. Your therapist might use your own stairs for gait training or your kitchen counter for standing balance exercises, making every session directly applicable to your daily life.
Occupational therapists focus on the practical skills you need for independence. They assess how stroke has affected your ability to dress, cook, bathe, or manage medications. Rather than generic exercises, they guide you through actual tasks in your own bathroom or kitchen, identifying barriers and teaching compensatory strategies. This role of home rehabilitation becomes especially powerful when therapy happens where you actually live.
Speech therapists address communication difficulties and swallowing problems that commonly follow stroke. They evaluate your speech clarity, language comprehension, and ability to safely consume different food textures. Sessions might involve practicing conversations during family meals or working on word-finding strategies during everyday activities. The home context allows therapists to observe real communication challenges rather than artificial clinical scenarios.
Each therapist tailors interventions based on your stroke severity, affected body side, cognitive status, and personal priorities. A patient focused on returning to cooking receives different occupational therapy than someone prioritizing self-care. This customization explains why home rehabilitation for stroke often produces better functional outcomes than standardized hospital programs.
- Physical therapists address walking, transfers, balance, and strength using your actual home environment
- Occupational therapists work on dressing, bathing, cooking, and other daily tasks in your own spaces
- Speech therapists improve communication and swallowing through real-world practice situations
- All therapists coordinate care to address overlapping goals and maximize recovery efficiency
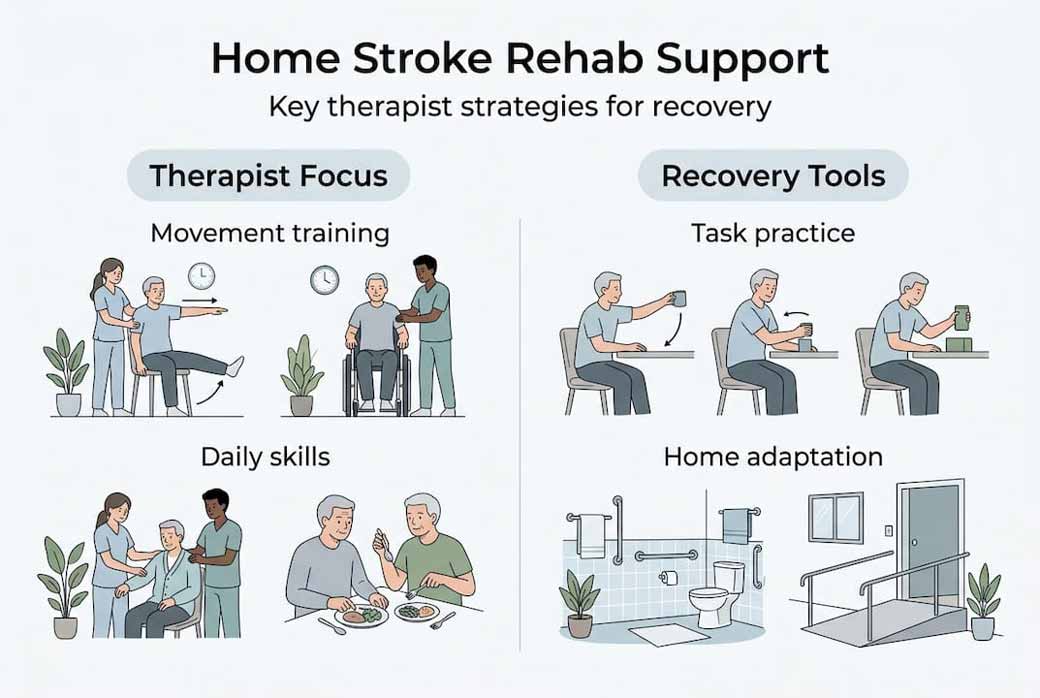
 How therapists enhance recovery through proven methods
How therapists enhance recovery through proven methods
Therapists apply evidence-based techniques grounded in how your brain recovers after injury. Task-specific training, constraint-induced movement therapy, mirror therapy, and neuroplasticity-based intensive practice have all demonstrated measurable improvements in motor function. Understanding these methods helps you engage more actively in your recovery.
Neuroplasticity, your brain’s ability to reorganize and form new neural connections, drives all effective rehabilitation. When you repeatedly practice a movement or task, you strengthen the brain pathways controlling that action. Therapists design exercises that challenge you at the right level, gradually increasing difficulty as your abilities improve. This progressive approach keeps your brain adapting without causing frustration or injury.
Task-specific training means practicing the exact activities you want to improve. If standing from a chair is difficult, your therapist has you practice that specific movement dozens of times per session rather than doing generic leg exercises. This direct approach produces faster functional gains because your brain learns the precise motor pattern you need for daily life.
Constraint-induced movement therapy involves restricting your stronger arm to force use of the affected limb. While this sounds counterintuitive, it prevents learned non-use, where your brain starts ignoring the weaker side. Therapists carefully supervise this technique, ensuring you practice functional tasks safely while building strength and coordination in the affected arm.
Mirror therapy uses visual feedback to trick your brain into perceiving movement in your affected limb. You watch your unaffected hand in a mirror while attempting to move the affected hand, creating the illusion of normal bilateral movement. This technique activates motor areas of your brain and can reduce pain while improving movement quality.
Intensity matters tremendously. Research on rehabilitation science basics shows that high repetition drives neuroplasticity more effectively than occasional practice. Your therapist structures sessions to maximize repetitions while managing fatigue, often incorporating rest breaks and varying activities to maintain engagement.
- Neuroplasticity principles guide all effective therapy by promoting brain reorganization through repeated practice
- Task-specific training produces faster functional gains than generic exercise programs
- High-intensity, repetitive practice accelerates motor recovery when properly supervised
- Therapists adjust difficulty progressively to challenge your abilities without causing frustration
Pro Tip: Keep a simple log of your practice between therapy sessions. Recording repetitions and noting which tasks feel easier helps your therapist adjust your program and shows you tangible progress during challenging recovery phases.
The rehabilitation exercise guide your therapist provides should include specific repetition targets and clear instructions for home practice. Consistency between supervised sessions determines how quickly you regain function.
Assessing and adapting the home environment for effective rehab
Therapists conduct thorough home evaluations to identify safety hazards and opportunities for environmental modifications. Home assessments examine fall risks, recommend safety modifications, guide caregiver training, and establish monitoring systems to track your functional progress. This proactive approach prevents injuries while creating conditions that support independent function.
The assessment process follows a systematic approach:
- Therapists walk through your home, observing how you navigate doorways, stairs, and furniture arrangements
- They identify specific hazards like loose rugs, poor lighting, or bathroom grab bar needs
- They evaluate whether your current furniture height and placement support safe transfers and mobility
- They recommend adaptive equipment such as shower benches, raised toilet seats, or reacher tools
- They train family members on proper assistance techniques to prevent caregiver injuries
- They establish baseline measurements of your functional abilities to track improvement over time
Common modifications dramatically reduce fall risk while promoting independence. Removing throw rugs eliminates tripping hazards. Installing grab bars in bathrooms provides stability during transfers. Rearranging furniture creates wider pathways for walkers or wheelchairs. These simple changes make your home a therapeutic environment rather than an obstacle course.

Caregiver training forms a critical component of home rehabilitation success. Therapists teach family members proper transfer techniques, exercise supervision methods, and strategies to engage patients in rehab between formal sessions. This education ensures consistent support and prevents well-meaning helpers from inadvertently hindering your recovery by doing too much for you.
Progress monitoring happens through regular reassessment of functional abilities. Your therapist tracks improvements in walking distance, balance scores, self-care independence, and other measurable outcomes. This data guides treatment adjustments and helps insurance justify continued therapy services. The rehabilitation workflow for patients includes clear documentation of these functional gains.
| Assessment Area | Typical Modifications | Expected Outcome |
|---|---|---|
| Bathroom safety | Grab bars, shower bench, raised toilet seat | Reduced fall risk, increased bathing independence |
| Mobility pathways | Furniture rearrangement, rug removal, improved lighting | Safer navigation, reduced fall anxiety |
| Kitchen access | Lowered storage, adaptive utensils, stable seating | Increased meal preparation participation |
| Bedroom setup | Bed height adjustment, bedside commode, clear floor space | Safer nighttime mobility, better sleep quality |
Pro Tip: Take photos of your home setup before therapy starts. Comparing these images to your modified environment months later provides powerful visual evidence of how environmental changes supported your functional gains.
Challenges and tailoring therapy for complex cases in home rehab
Not all stroke recoveries follow a smooth path. Severe strokes and socioeconomic factors complicate rehabilitation, requiring therapists to adapt their approaches significantly. Understanding these challenges helps you set realistic expectations while working with your therapy team to overcome obstacles.
Stroke severity dramatically affects recovery trajectory. Patients with mild strokes often regain independence quickly with minimal intervention. Moderate to severe strokes require intensive, prolonged therapy with careful attention to preventing complications like contractures or pressure sores. Your therapist adjusts treatment intensity, duration, and goals based on your specific impairment level.
Fatigue presents a major barrier to consistent practice. Neurological fatigue differs from normal tiredness because it results from your brain working harder to accomplish basic tasks. Therapists structure sessions with strategic rest breaks and vary activities to maintain engagement without overwhelming you. They also educate you on energy conservation techniques to maximize function throughout the day.
 Socioeconomic factors influence access to therapy services, equipment, and caregiver support. Therapists working with limited resources become creative problem solvers, using household items as exercise equipment and identifying community resources for financial assistance. They prioritize interventions that provide maximum functional benefit within available session limits.
Socioeconomic factors influence access to therapy services, equipment, and caregiver support. Therapists working with limited resources become creative problem solvers, using household items as exercise equipment and identifying community resources for financial assistance. They prioritize interventions that provide maximum functional benefit within available session limits.
Chronic phase recovery requires different strategies than acute rehabilitation. Months or years after stroke, traditional therapy services often end despite continued potential for improvement. Therapists in this phase focus on teaching self-directed exercise programs, connecting you with community fitness resources, and addressing new challenges that emerge as you attempt more complex activities.
Family dynamics significantly impact adherence to home programs. Therapists navigate situations where caregivers feel overwhelmed, family members disagree on care approaches, or patients resist assistance. Building strong therapeutic alliances and providing emotional support alongside physical interventions becomes essential for long-term success.
- Severe strokes require intensive, prolonged therapy with modified expectations for functional outcomes
- Neurological fatigue necessitates strategic rest breaks and energy conservation education
- Limited resources prompt creative use of household items and community support networks
- Chronic phase recovery focuses on self-directed programs and addressing emerging challenges
- Family dynamics require therapists to provide emotional support and conflict resolution strategies
| Challenge Type | Therapist Strategy | Patient/Caregiver Action |
|---|---|---|
| Severe impairment | Intensive repetition, adaptive equipment, realistic goal setting | Commit to consistent practice, celebrate small gains |
| Fatigue management | Strategic rest breaks, energy conservation techniques | Track energy patterns, prioritize essential activities |
| Limited resources | Household item exercises, community resource referrals | Explore financial assistance programs, join support groups |
| Chronic phase plateau | Self-directed programs, community fitness integration | Maintain exercise routine, seek new challenges |
Structured interventions combined with family support improve adherence even in complex cases. When you understand why specific exercises matter and how they connect to your personal goals, you engage more consistently. Therapists who take time to explain the science behind their recommendations and celebrate your progress build the motivation necessary for long-term commitment.
The connection between how rehab improves mobility and these individualized approaches becomes clear when you see therapists adjusting techniques based on your responses. Following physical therapy best practices means constantly evaluating what works for your unique situation rather than applying cookie-cutter protocols.
Discover tools to support your home rehabilitation journey
While therapist expertise drives your recovery, specialized equipment can amplify your progress between sessions. Tisele Rehab offers innovative rehabilitation kits for stroke recovery designed specifically for home use, complementing the work you do with your therapy team.
These tools include the FitMi system, which uses engaging exercises to promote high-repetition practice that builds on neuroplasticity principles your therapist emphasizes. The MusicGlove combines hand therapy with music-based activities, making repetitive finger exercises more enjoyable and sustainable. Browse rehabilitation aids that address specific functional challenges your therapist has identified, from mobility support to daily living adaptations. The home neurorehabilitation system integrates seamlessly with therapist-prescribed programs, giving you structured practice options when working independently. These evidence-based solutions help you maintain the intensity and consistency that drive meaningful functional improvements.
FAQ
What types of therapists are involved in home rehabilitation?
Three main therapist types support home stroke recovery. Physical therapists address mobility, balance, and strength needed for walking and transfers. Occupational therapists focus on daily living skills like dressing, bathing, and cooking, helping you regain independence in self-care and household tasks. Speech therapists work on communication difficulties and swallowing problems that commonly follow neurological injuries. Each professional brings specialized assessment tools and treatment techniques, and they coordinate care to address your complete recovery needs rather than working in isolation. The role of home rehabilitation becomes most effective when these disciplines collaborate around your specific goals and home environment.
How does home rehabilitation compare to hospital rehab after stroke?
Home-based rehabilitation produces comparable outcomes to hospital programs while offering distinct advantages. You practice functional tasks in the environment where you actually need those skills, making the transfer of learning more direct. Therapists observe real-world challenges like navigating your specific bathroom layout or managing your actual kitchen setup, allowing for more targeted problem-solving. Home settings also reduce infection risks and provide the comfort of familiar surroundings, which can improve motivation and reduce anxiety. The key factor determining effectiveness is therapist involvement and program structure rather than location. Home rehabilitation for stroke works best when you receive adequate therapy frequency and intensity, not as a lower-quality alternative to hospital care.
What can caregivers do to support successful home rehab?
Caregivers play an essential role in rehabilitation success. Caregiver training and involvement boost therapy adherence significantly by providing continuity between formal therapy sessions. Therapists teach you proper assistance techniques that promote patient independence rather than creating dependence. You learn exercise supervision methods, safety strategies, and ways to engage patients in rehab during daily activities. Emotional support matters tremendously, as recovery involves setbacks and frustration. Celebrating small victories, maintaining optimism during plateaus, and helping patients see incremental progress keeps motivation high. Caregivers also serve as communication bridges, helping therapists understand what challenges arise between sessions and advocating for program adjustments when needed.
Recommended
38
Get inspired by a stroke recovery story
Home rehabilitation at full speed.
My husband suffered a severe stroke on August 19, 2020, which paralyzed him on the right side. Thanks to FitMi he has made huge progress since then. He still has no strength in his right arm, but now he can walk with a cane, his speech has improved significantly, and he is fighting and rehabilitating at full speed. We are very happy that we bought this FitMi kit for him, so he can continue his training and exercises at home. We are encouraged by this program and the positive reviews we read from others who used it. Thank God we found this kit and thank you for your support. It is a wonderful program.
Kate (08.09.2020)








