Neurological rehab terminology: patient guide 2026
You sit in a therapy session and hear terms like neuroplasticity, hemiparesis, and central pattern generators. The therapist speaks confidently, but you feel lost. Understanding neurological rehabilitation terminology isn’t just about decoding medical jargon; it’s about taking control of your recovery journey. When you grasp what these terms mean, you can ask better questions, track progress more effectively, and collaborate with your care team to optimize outcomes. This guide translates complex rehab vocabulary into plain language, empowering you and your caregivers to navigate neurological recovery with confidence and clarity.
Table of Contents
- Key takeaways
- Basic neurological rehab terms patients should know
- Core neurological rehabilitation therapies and approaches
- Empirical benchmarks and understanding recovery progress
- Nuances, challenges, and practical advice for patients and caregivers
- Explore rehabilitation kits and aids to support your neurological recovery
- FAQ
Key Takeaways
| Point | Details |
|---|---|
| Basic rehab terms | Knowing terms like agnosia and hemiparesis helps you understand therapy conversations and ask more precise questions. |
| Core rehab therapies | Core therapies include task specific training bilateral movement training CIMT virtual reality robotic assisted therapy and FES as central approaches. |
| Active participation | Recognizing terms helps you identify targeted deficits and understand why specific exercises matter in your plan. |
| Proactive note taking | Keep a small notebook during therapy sessions to jot unfamiliar terms and review them later with your therapist. |
 Basic neurological rehab terms patients should know
Basic neurological rehab terms patients should know
When your therapist mentions agnosia during an evaluation, it helps to know they’re describing difficulty recognizing familiar objects or people, not a personality change. Neurorehabilitation glossaries define key terms that appear repeatedly in recovery conversations. Hemiparesis refers to weakness on one side of your body, a common consequence of stroke that affects movement and coordination. Neuroplasticity describes your brain’s remarkable ability to rewire itself, forming new neural connections to compensate for damaged areas.
Activities of Daily Living, or ADLs, encompass basic self-care tasks like dressing, bathing, and eating that therapists use to measure functional independence. Central Pattern Generators are neural networks in your spinal cord that coordinate rhythmic movements like walking, which rehabilitation exercises aim to reactivate. These foundational concepts appear in almost every therapy plan, assessment report, and progress discussion.
Understanding rehabilitation science basics transforms passive participation into active collaboration. When you recognize these terms, you can identify which specific deficits your therapy targets and why certain exercises matter more than others. Additional patient-friendly definitions help clarify terminology that initially seems overwhelming.
Here are essential terms you’ll encounter frequently:
- Agnosia: Inability to recognize objects, people, sounds, or smells despite intact sensory function
- Hemiparesis: Weakness affecting one side of the body, ranging from mild to severe
- Neuroplasticity: The brain’s capacity to reorganize neural pathways based on experience and practice
- ADLs: Fundamental self-care activities that measure functional independence
- Central Pattern Generators: Spinal cord circuits that produce rhythmic motor patterns
- Proprioception: Your sense of body position and movement in space
- Spasticity: Increased muscle tone causing stiffness and involuntary contractions
Pro Tip: Keep a small notebook during therapy sessions to jot down unfamiliar terms. Look them up afterward and ask your therapist to explain how they apply to your specific recovery plan. This practice builds your rehab vocabulary quickly and helps you participate more actively in treatment decisions.
Core neurological rehabilitation therapies and approaches
Task-specific training forms the backbone of modern neurorehabilitation, focusing on practicing actual movements you want to regain rather than generic exercises. If you struggle with buttoning shirts, your therapist designs activities that mimic that precise motion, gradually increasing difficulty as your dexterity improves. This approach leverages neuroplasticity by repeatedly activating the exact neural pathways needed for real-world function.
Bilateral movement training involves using both arms or legs simultaneously, helping the unaffected side guide the impaired side through movements. Constraint-Induced Movement Therapy (CIMT) takes the opposite approach, restricting your stronger limb to force intensive use of the weaker one. Core therapies include task-specific training, bilateral movement training, CIMT, VR, robotic-assisted therapy, and FES, each targeting different recovery mechanisms.

Advanced technologies expand therapeutic possibilities beyond traditional hands-on approaches. Virtual reality immerses you in engaging environments where repetitive practice feels like gaming rather than tedious exercise. Robotic-assisted therapy provides precisely controlled resistance and support, enabling movement patterns you couldn’t achieve independently. Functional Electrical Stimulation (FES) delivers targeted electrical pulses to muscles, triggering contractions that retrain motor control.
Common therapy types you might encounter include:
- Task-specific training: Practicing functional movements relevant to daily activities
- Bilateral movement training: Coordinating both limbs simultaneously to enhance neural activation
- Constraint-Induced Movement Therapy: Restricting the stronger limb to promote weaker limb use
- Virtual reality therapy: Using immersive technology to motivate repetitive practice
- Robotic-assisted therapy: Leveraging machines for precise movement guidance and support
- Functional Electrical Stimulation: Applying electrical currents to stimulate muscle contractions
Recent advancements emphasize tech-based and human-intensive approaches yielding equivalent outcomes when properly implemented. The choice between approaches depends on your specific impairments, available resources, and personal preferences rather than one being universally superior.
| Approach Type | Primary Focus | Resource Requirements | Typical Outcomes |
|---|---|---|---|
| Human-Intensive | Hands-on guidance, manual resistance, personalized feedback | Skilled therapists, time-intensive sessions | Equivalent functional gains with high engagement |
| Technology-Dependent | Robotic assistance, VR environments, FES devices | Equipment investment, technical setup | Equivalent functional gains with consistent protocols |
Exploring top rehabilitation exercises and understanding rehab technology for stroke recovery helps you appreciate how different modalities complement each other. Some patients respond better to technology-driven approaches, while others thrive with traditional hands-on therapy.
Pro Tip: Don’t assume newer technology automatically means better results. Match therapy type to your specific needs, motivation style, and access to resources. A motivated patient with consistent home practice often outperforms someone with cutting-edge equipment but inconsistent effort.
Empirical benchmarks and understanding recovery progress
The Fugl-Meyer Assessment - Upper Extremity (FMA-UE) serves as the gold standard for measuring stroke recovery, scoring motor function from 0 to 66 points. FMA-UE scores generally improve about 10 points at 4 weeks, 12 at 12 weeks, and 16 at 24 weeks post-stroke with standard care. A gain of 5 to 10 points represents the Minimal Clinically Important Difference (MCID), meaning you’ll notice meaningful functional improvements in daily activities.
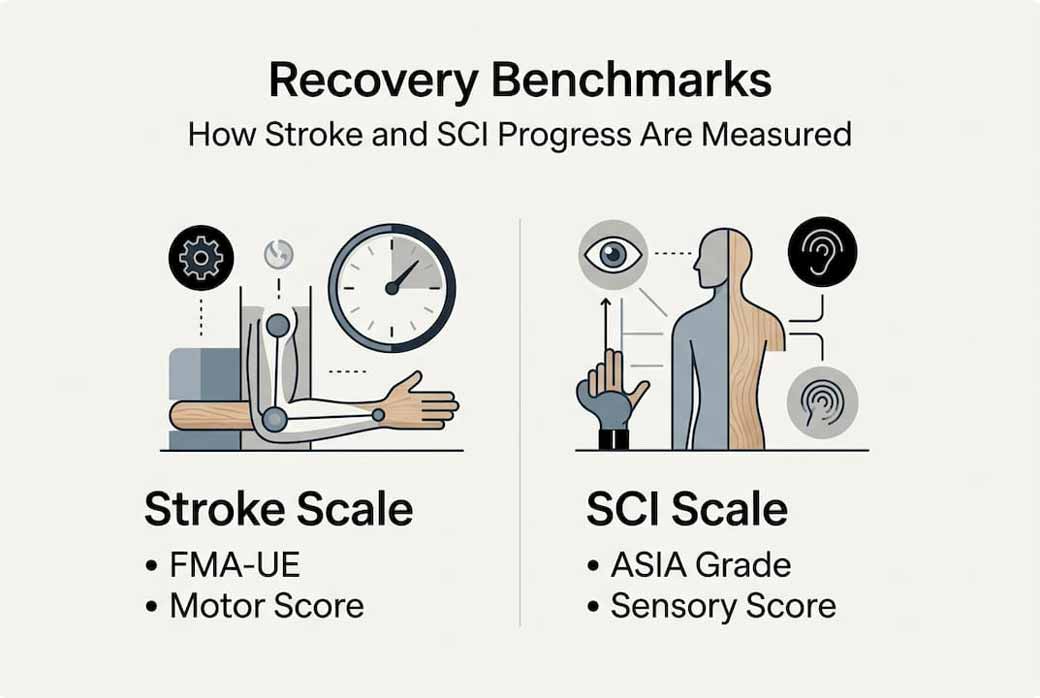
Spinal cord injury (SCI) recovery uses the ASIA Impairment Scale, grading from A (complete) to E (normal). Moving from ASIA B to C, or C to D, signifies substantial motor function return that translates to increased independence. Traumatic brain injury (TBI) outcomes are tracked through measures like the Functional Independence Measure (FIM), which scores self-care, mobility, and cognitive abilities.
SCI rehabilitation outcomes show typical improvement patterns during inpatient rehab, though individual trajectories vary widely based on injury level and completeness. Understanding these benchmarks helps you set realistic expectations while staying motivated through plateaus.
| Condition | Typical Timeline | Expected Progress | Measurement Tool |
|---|---|---|---|
| Stroke (Upper Extremity) | 4-24 weeks | 10-16 point FMA-UE gain | Fugl-Meyer Assessment |
| Spinal Cord Injury | 3-6 months inpatient | 1-2 ASIA grade improvement | ASIA Impairment Scale |
| Traumatic Brain Injury | 2-6 months acute rehab | 20-40 point FIM increase | Functional Independence Measure |
| Stroke (Lower Extremity) | 6-12 weeks | Gait speed increase 0.1-0.3 m/s | 10-Meter Walk Test |
Several factors influence whether you’ll exceed or fall short of these benchmarks:
- Therapy intensity: More frequent, longer sessions typically produce faster gains
- Patient engagement: Active participation and home practice accelerate progress
- Injury severity: Milder impairments generally recover more quickly and completely
- Time since injury: Earlier intervention often yields better outcomes
- Comorbidities: Other health conditions can slow rehabilitation progress
- Social support: Strong caregiver involvement enhances adherence and motivation
“Recovery isn’t linear. You might gain 8 points in the first month, plateau for weeks, then suddenly jump another 5 points. The brain reorganizes in bursts, not steady increments.”
Understanding rehabilitation outcomes and motor scores helps you interpret your progress accurately. Recovery means regaining original movement patterns through neural repair, while compensation involves learning alternative strategies to accomplish tasks despite persistent impairments. Both are valuable, but distinguishing between them helps you and your therapist adjust treatment focus as recovery evolves.
 Nuances, challenges, and practical advice for patients and caregivers
Nuances, challenges, and practical advice for patients and caregivers
Learned helplessness develops when repeated failed attempts convince you that effort won’t improve outcomes, leading to passive withdrawal from therapy. Learned non-use occurs when you unconsciously favor your stronger side even after regaining some function in the weaker limb, preventing further neural recovery. Sex influences technology outcomes; learned non-use and maladaptive plasticity are critical challenges that intensive protocols must address.
Maladaptive plasticity represents the brain’s dark side, where neural reorganization reinforces abnormal movement patterns or pain signals rather than functional recovery. Spasticity can worsen through maladaptive changes if not managed properly, creating a cycle of increasing dysfunction. Breaking these patterns requires intensive, properly structured therapy that promotes beneficial neural rewiring.
Research reveals sex differences in responses to virtual reality and robotic therapies, with women sometimes showing different engagement patterns and outcomes compared to men. These findings suggest that one-size-fits-all protocols may not optimize results for all patients, highlighting the importance of personalized treatment approaches.
The recovery versus compensation debate shapes therapeutic philosophy and patient expectations. Recovery vs compensation debate affects therapy direction and patient expectations significantly. Some therapists prioritize true recovery of original movement patterns, while others emphasize compensation strategies that restore function through alternative methods. Neither approach is inherently superior; the optimal balance depends on your specific impairments, recovery stage, and functional goals.
Common challenges patients and caregivers face include:
- Information overload: Too many unfamiliar terms introduced simultaneously
- Inconsistent terminology: Different providers using varied terms for similar concepts
- Unrealistic expectations: Misunderstanding benchmarks leading to discouragement
- Communication barriers: Difficulty expressing concerns or asking clarifying questions
- Resource constraints: Limited access to specialized therapies or equipment
- Caregiver burnout: Overwhelming demands without adequate support systems
Pro Tip: Schedule brief check-ins with your therapist specifically to discuss terminology and progress interpretation. Don’t wait until you’re confused or frustrated. Proactive communication prevents misunderstandings that can derail motivation and adherence.
Caregivers play a crucial role in bridging terminology gaps and reinforcing therapy principles at home. When professional therapy sessions are limited by insurance or geography, family members who understand rehab concepts can facilitate continued progress through guided home practice. Learning rehab and mobility improvements and strategies for patient engagement in rehab equips caregivers to provide meaningful support beyond basic assistance.
Integrating family support requires clear communication about which activities promote recovery versus those that merely compensate. Well-meaning caregivers sometimes inadvertently reinforce learned non-use by doing too much for patients, preventing opportunities for therapeutic struggle that drives neuroplasticity. Understanding terminology helps caregivers recognize when to assist and when to encourage independent effort.
Explore rehabilitation kits and aids to support your neurological recovery
Now that you understand neurological rehab terminology and concepts, you can make informed decisions about tools that support your recovery journey. Tisele Rehab specializes in rehabilitation aids designed specifically for stroke, cerebral palsy, and other neurological conditions. These products translate the therapeutic principles you’ve learned into practical home-based solutions.
The FitMi home neurorehabilitation system exemplifies task-specific training through engaging, gamified exercises that promote neuroplasticity. You can practice the repetitive movements your brain needs to rewire, tracking progress with the same evidence-based principles used in clinical settings. MusicGlove combines bilateral movement training with motivating music-based activities, making hand therapy feel less like work and more like play.
Tisele Rehab rehabilitation kits bundle complementary tools that address multiple aspects of neurological recovery, from motor function to cognitive engagement. These systems work seamlessly at home while remaining compatible with clinical protocols, ensuring consistency across all your therapy environments. Whether you’re working on upper extremity function, gait training, or fine motor skills, understanding the terminology behind these approaches helps you maximize their benefits and communicate effectively with your care team about your home practice.
FAQ
What is neuroplasticity and why is it important in rehab?
Neuroplasticity is your brain’s ability to reorganize neural connections by forming new pathways in response to learning, experience, or injury. In rehabilitation, targeted exercises exploit this capacity to help undamaged brain regions assume functions previously controlled by injured areas. Understanding neuroplasticity in stroke recovery explains why repetitive, intensive practice produces better outcomes than passive treatments. The more you practice specific movements, the stronger these new neural pathways become, gradually restoring function.
How can patients track their neurological recovery progress?
Clinical scales like the Fugl-Meyer Assessment provide standardized measurements that therapists use to quantify motor improvements over time. You can also track functional gains by noting improvements in daily activities such as dressing speed, walking distance, or hand dexterity during meals. Tracking rehabilitation outcomes helps you recognize progress that might feel incremental day-to-day but becomes substantial over weeks. Regular therapy feedback combined with personal observations creates a complete picture of your recovery trajectory.
What are common psychological barriers impacting neurological rehab?
Learned helplessness occurs when repeated failures convince you that effort won’t improve outcomes, leading to reduced participation in therapy. Learned non-use develops when you unconsciously avoid using a recovering limb because compensating with your stronger side feels easier. Both barriers require intensive protocols and deliberate practice to overcome, as passive approaches reinforce these maladaptive patterns. Understanding psychological barriers in rehab helps you recognize when these patterns emerge so you can address them proactively with your care team.
How do technology-based therapies differ from traditional neurorehabilitation?
Technology-based approaches like virtual reality and robotic-assisted therapy provide precise, consistent movement guidance and engaging feedback that can increase practice volume. Traditional hands-on therapy offers personalized tactile cues and real-time adjustments based on therapist expertise. Research shows both methods produce equivalent outcomes when protocols are properly designed and consistently applied. Technology-based neurorehab works best when matched to individual patient preferences, available resources, and specific impairment patterns rather than assuming one approach universally outperforms the other.
Recommended
38
Zainspiruj się historią powrotu do zdrowia po udarze mózgu
Moja opinia o MusicGlove
Oto moja krótka opinia - recenzja MusicGlove. 3 października 2020 r. przeszedłem udar krwotoczny mózgu. Kupiłem MusicGlove po około 4 miesiącach hospitalizacji. Mogłem wtedy poruszać palcami, ale - delikatnie mówiąc - "niezbyt" skutecznie. Prawdę mówiąc, nie potrafiłem chwytać małych przedmiotów, takich jak długopis czy drobne rzeczy, i pisałem tylko zdrową ręką. Dwa miesiące użytkowania. Potrafię już trochę pisać - krótko, bo krótko - ale mogę już napisać coś moją niesprawną ręką, co mnie uspokaja i daje nadzieję na powrót do pracy. Nie stanie się to od razu, jednak ta myśl popycha mnie do przodu i mam teraz jasny i realistyczny cel. Jedynym minusem jest może ograniczona liczba piosenek. Więc muzyka czasami się powtarza. Aha!... Upewnijcie się, że macie odpowiednią rękawicę - właściwy rozmiar - nie może być ani za duża, ani za mała! Zamówiłem rozmiar, który okazał się za duży, ale obsługa klienta była doskonała i szybka, sprawnie i szybko wymienili mi rozmiar. Zestaw jest łatwy w instalacji, dosłownie "podłącz i używaj". Podsumowując: Brawo dla mnie i Brawo dla TiSale Rehab.
Nikodem (24.02.2021)