Understanding neuro rehab outcomes: 2026 guide
Recovering from a stroke involves far more than regaining physical movement. Many survivors and their caregivers focus solely on motor skills, overlooking cognitive, emotional, and social recovery dimensions that profoundly shape independence and quality of life. Neurorehabilitation addresses this complexity by targeting multiple recovery pathways simultaneously, from retraining neural circuits to adapting daily routines. Understanding what constitutes meaningful outcomes and how innovative therapies accelerate progress empowers you to make informed decisions about your recovery journey. This guide clarifies the multifaceted nature of neurorehabilitation outcomes and explores evidence-based strategies that support holistic healing.
Table of Contents
- Understanding Neurorehabilitation Outcomes: Dimensions And Importance
- Advanced Therapies And Tools Boosting Neurorehab Outcomes
- Caregiver Role And Holistic Approach To Improving Neurorehabilitation Outcomes
- Practical Strategies To Maximize Neurorehab Outcomes At Home And Beyond
- Enhance Your Neurorehabilitation Journey With Tisele Rehab
- Frequently Asked Questions
Key takeaways
| Point | Details |
|---|---|
| Multidimensional recovery | Neurorehabilitation targets motor, cognitive, sensory, emotional, and social functions beyond physical movement alone. |
| Independence and quality | Effective outcomes restore daily living abilities and enhance overall life satisfaction after stroke. |
| Innovative tools accelerate progress | Advanced therapies like robot-assisted training and adaptive stimulation optimize neuroplasticity when applied correctly. |
| Caregiver involvement matters | Active participation improves patient adherence but requires balanced support to prevent caregiver burnout. |
| Intensive rehab yields results | Customized high-intensity protocols can produce meaningful recovery even years post-stroke. |
 Understanding neurorehabilitation outcomes: dimensions and importance
Understanding neurorehabilitation outcomes: dimensions and importance
Neurorehabilitation aims to improve function, independence, and quality of life after nervous system damage by retraining the brain and adapting to daily tasks. This process goes beyond simple physical therapy. It encompasses a comprehensive approach that addresses every aspect of how stroke affects your life. The brain’s remarkable ability to reorganize itself, known as neuroplasticity, forms the foundation of effective rehabilitation.
Recovery differs fundamentally from compensation. True recovery means regaining lost abilities through neural repair and reorganization. Compensation involves learning alternative strategies to accomplish tasks despite persistent impairments. Both pathways contribute to improved outcomes, but understanding this distinction helps set realistic expectations and choose appropriate therapies.
Recovery includes motor/physical, sensory/perceptual, cognitive, affective, and psychosocial dimensions. Each dimension influences your ability to live independently and engage meaningfully with your environment:
- Motor and physical recovery restore movement control, strength, coordination, and endurance for walking, reaching, and manipulating objects
- Sensory and perceptual recovery rebuild touch sensation, spatial awareness, and visual processing critical for safe navigation
- Cognitive recovery addresses attention, memory, problem solving, and executive functions needed for decision making
- Affective recovery manages emotional regulation, motivation, and mental health challenges like post-stroke depression
- Psychosocial recovery reconnects you with relationships, community participation, and valued life roles
Successful neurorehabilitation outcomes require simultaneous progress across these dimensions. A stroke survivor who regains walking ability but struggles with depression and social isolation experiences limited quality of life improvements. Similarly, cognitive deficits can undermine physical therapy adherence, while sensory impairments increase fall risk despite adequate strength.
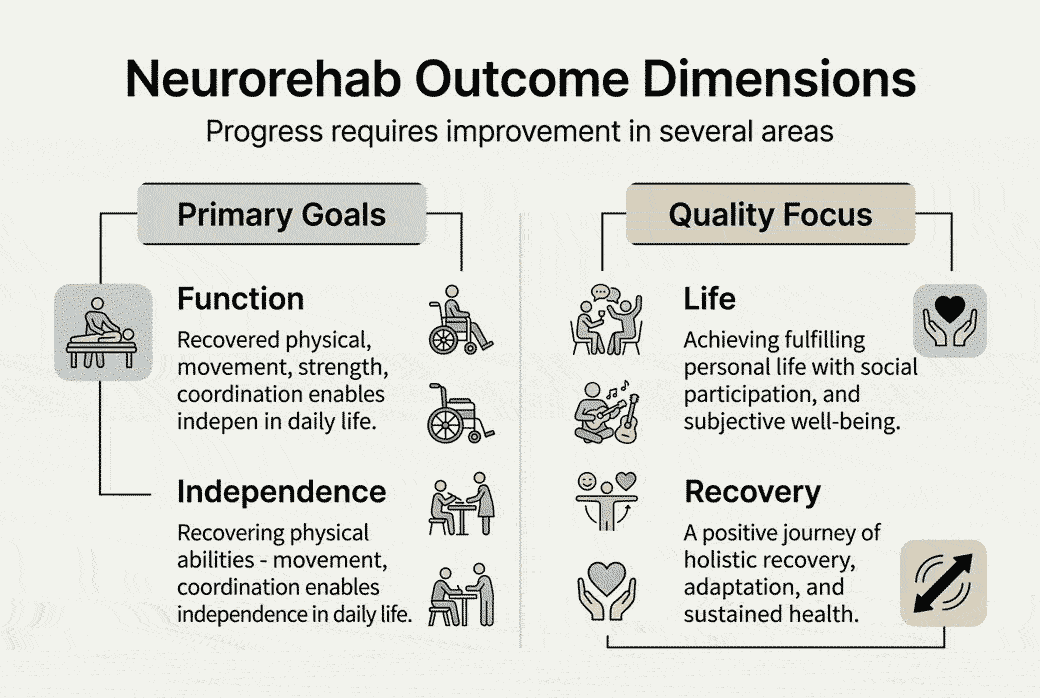
The complexity of targeting multiple recovery areas simultaneously demands coordinated, individualized treatment plans. Your rehabilitation team must assess each dimension, identify priorities based on your goals, and design interventions that address interconnected challenges. This holistic perspective ensures that therapy efforts translate into meaningful improvements in daily independence and life satisfaction.
Advanced therapies and tools boosting neurorehab outcomes
Modern neurorehabilitation leverages evidence-based therapies and innovative technologies to optimize recovery potential. Resistance training and robot-assisted therapy are most effective for enhancing walking capacity after stroke. These methods harness neuroplasticity principles by providing intensive, repetitive practice that drives neural reorganization.
Several therapy approaches have demonstrated superior outcomes in clinical trials:
- Resistance training builds muscle strength and endurance through progressive weight-bearing exercises
- Robot-assisted therapy delivers consistent, high-repetition movement practice with adjustable support levels
- Constraint-induced movement therapy (CIMT) and task-specific training improve upper limb motor function by restricting the unaffected limb and practicing functional activities
- Task-specific training focuses practice on real-world activities you need to perform independently
Clinical measurements like the 6-minute walk test and 10-meter walk test quantify mobility improvements objectively. These standardized assessments help track progress and adjust therapy intensity. Studies show that patients receiving robot-assisted gait training combined with conventional therapy achieve significantly greater walking speed and endurance compared to conventional therapy alone.
Cutting-edge technology continues expanding rehabilitation possibilities. The Magnetic NeuroRing enables adaptive transcranial magnetic stimulation to improve motor dysfunction post-stroke by combining EEG monitoring with targeted brain stimulation. This device adjusts stimulation parameters in real time based on your brain activity patterns, optimizing neuroplasticity effects.

Mirror therapy and virtual reality offer supplementary benefits, though research shows heterogeneous results across different patient populations. Mirror therapy creates visual feedback that tricks the brain into perceiving movement in the affected limb. Virtual reality immerses you in engaging environments that motivate repetitive practice while providing immediate performance feedback.
Pro Tip: Consistency and tailored intensity in using these therapies maximize neuroplasticity effects. Aim for daily practice sessions that challenge your current abilities without causing excessive fatigue or frustration.
The following table compares leading therapy methods:
| Therapy Method | Primary Benefits | Ideal Use Cases |
|---|---|---|
| Resistance Training | Builds strength and endurance for functional activities | Lower limb weakness, reduced walking capacity |
| Robot-Assisted Therapy | Provides high-repetition practice with adjustable support | Severe motor impairment, early recovery stages |
| CIMT | Forces use of affected limb to overcome learned non-use | Upper limb recovery with some voluntary movement |
| Task-Specific Training | Practices real-world activities directly | All recovery stages, customized to individual goals |
| Magnetic NeuroRing | Adaptive brain stimulation targeting neural circuits | Motor dysfunction responsive to neuromodulation |
Integrating multiple therapy modalities creates synergistic effects. For example, combining resistance training with task-specific practice builds both the physical capacity and skilled coordination needed for independence. Home rehabilitation extends therapy benefits beyond clinical sessions, allowing you to accumulate the intensive practice hours that drive motor recovery.
Caregiver role and holistic approach to improving neurorehabilitation outcomes
Caregivers play an indispensable role in neurorehabilitation success. They provide emotional support, assist with exercise programs, monitor safety, and help maintain therapy schedules between clinical appointments. Active caregiver participation improves patient adherence and outcomes but increases caregiver stress and psychological strain. This dual reality requires balanced approaches that optimize patient recovery while protecting caregiver wellbeing.
Caregivers contribute to recovery in multiple ways:
- Encouraging consistent therapy participation and celebrating incremental progress
- Assisting with home exercise programs and ensuring proper technique
- Monitoring for complications, medication side effects, and emotional changes
- Facilitating communication between the patient and healthcare team
- Adapting the home environment to support safety and independence
The psychological burden caregivers face should not be underestimated. Witnessing a loved one struggle with basic tasks, managing complex care routines, and adjusting to role changes creates significant stress. Many caregivers experience depression, anxiety, social isolation, and physical health decline. Addressing caregiver needs directly improves both caregiver and patient outcomes.
Holistic rehabilitation recognizes the patient-caregiver dyad as the fundamental unit of recovery. Effective programs incorporate:
- Cultural adaptation of therapy approaches to align with family values and communication styles
- Psychosocial support addressing emotional needs, relationship dynamics, and community reintegration
- Intensive protocols that balance high practice volumes with sustainable routines
- Education empowering both patients and caregivers to understand recovery processes and set realistic goals
Cross-continental validation shows equivalent rehab outcomes when intensity and neuroplasticity targeting are consistent, highlighting human expertise importance. Technology enhances therapy delivery but does not replace skilled clinicians who assess individual needs, adjust interventions, and provide the human connection that motivates continued effort.
Caregivers can support recovery while managing their own wellbeing by following these steps:
- Establish clear boundaries around caregiving responsibilities and personal time for rest and self-care activities.
- Join caregiver support groups to share experiences, learn coping strategies, and reduce isolation.
- Communicate openly with healthcare providers about challenges and request resources like respite care or counseling.
- Prioritize your own physical health through adequate sleep, nutrition, and medical care.
- Accept help from family, friends, and community resources rather than trying to manage everything alone.
Pro Tip: Seek caregiver support resources and incorporate psychosocial elements in recovery plans. Many rehabilitation centers offer caregiver education programs and support groups specifically designed for stroke families.
Essential rehabilitation tips from clinicians emphasize the importance of addressing both patient and caregiver needs as interconnected components of successful recovery. When caregivers feel supported and equipped with practical strategies, they become more effective partners in the rehabilitation process.
 Practical strategies to maximize neurorehab outcomes at home and beyond
Practical strategies to maximize neurorehab outcomes at home and beyond
Intensity and consistency drive neuroplasticity effectiveness at any recovery stage. Intensive neuroplasticity-driven rehab can achieve meaningful motor recovery years post-stroke without expensive technology. The brain retains capacity for reorganization long after initial injury, provided you supply sufficient stimulation through targeted practice.
Home-based rehabilitation extends therapy benefits by allowing daily high-repetition practice in your natural environment. This approach offers several advantages over clinic-only therapy:
- Greater total practice volume accumulated over weeks and months
- Immediate application of skills to real-world tasks and environments
- Reduced transportation barriers and scheduling constraints
- Lower costs compared to extended outpatient therapy
- Increased sense of control and ownership over the recovery process
Implement these steps to integrate effective therapy at home:
- Work with your clinician to design a customized home exercise program targeting your specific impairments and functional goals.
- Schedule dedicated practice times each day and treat them as non-negotiable appointments with yourself.
- Use adaptive equipment and technology to enable independent practice when caregiver assistance is unavailable.
- Track your performance on specific exercises and functional tasks to monitor progress and maintain motivation.
- Communicate regularly with your rehabilitation team to adjust exercises as your abilities improve or challenges emerge.
- Incorporate therapy principles into daily activities like dressing, cooking, and household tasks for additional practice opportunities.
The following table compares home-based neurorehabilitation tools:
| Tool/Device | Key Features | Primary Benefits |
|---|---|---|
| FitMi | Interactive exercises with real-time feedback and adaptive difficulty | Motivates high-repetition practice for upper and lower extremities |
| MusicGlove | Music-based hand therapy combining entertainment with therapeutic exercises | Improves hand function through engaging, game-like activities |
| Mirror Box | Simple visual feedback device for affected limb movement | Reduces pain and facilitates motor imagery for movement recovery |
| Tablet Apps | Cognitive training games and exercise tracking applications | Addresses attention, memory, and executive function deficits |
| Resistance Bands | Portable strength training equipment with variable resistance levels | Builds muscle strength and endurance for functional activities |
Overcoming learned helplessness requires both mental and physical engagement. Some stroke survivors develop a pattern of avoiding movement with the affected limb even when some function returns. This learned non-use perpetuates disability. Breaking this cycle demands deliberate practice that challenges you to use affected limbs in meaningful activities despite initial difficulty or discomfort.
Pro Tip: Customize routines and track progress to stay motivated and identify effective practices. Keep a simple log noting exercises completed, repetitions achieved, and functional improvements observed. This tangible record provides encouragement during plateaus and helps you recognize gradual gains that might otherwise go unnoticed.
Communicate regularly with your clinicians to adapt intensity and modalities as recovery evolves. What works during early recovery may need modification as you progress. Your therapy team can adjust exercise difficulty, introduce new techniques, and address emerging challenges. This ongoing collaboration ensures your home program remains optimally challenging and aligned with your changing needs.
Rehabilitation workflow for patients provides structured guidance on organizing daily therapy activities, balancing different exercise types, and integrating recovery efforts into your broader life context. Following evidence-based workflows helps you avoid common pitfalls like overtraining, neglecting important recovery dimensions, or losing motivation during extended recovery periods.
Enhance your neurorehabilitation journey with Tisele Rehab
Achieving optimal neurorehabilitation outcomes requires access to effective, engaging tools that support intensive practice at home and in clinical settings. Tisele Rehab specializes in rehabilitation kits for stroke and cerebral palsy designed to maximize recovery potential through innovative, evidence-based devices.
The MusicGlove hand rehabilitation device transforms repetitive hand therapy into an enjoyable musical experience. By combining therapeutic exercises with engaging gameplay, MusicGlove motivates the high-repetition practice essential for neuroplasticity. Similarly, the FitMi home neurorehabilitation system delivers interactive full-body exercises with real-time feedback and adaptive difficulty, enabling you to accumulate intensive practice hours that drive meaningful recovery.
These tools empower both patients and caregivers to take control of the rehabilitation process. Accessible technology removes barriers to consistent therapy while maintaining the intensity and engagement that produce results. Visit Tisele Rehab to explore tailored solutions supporting your unique recovery journey and discover how innovative devices can complement your rehabilitation program.
Frequently asked questions
What are the key factors that influence neurorehabilitation outcomes?
Therapy intensity, timing of intervention, patient motivation, caregiver involvement, and appropriate use of technology all significantly impact recovery. Early, intensive rehabilitation produces the best results, but meaningful gains remain possible years post-stroke with consistent, targeted practice. Individual factors like stroke severity, location, and pre-existing health conditions also affect recovery potential.
What is the difference between recovery and compensation in neurorehabilitation?
Recovery involves regaining lost abilities through neural repair and reorganization, restoring original movement patterns and functions. Compensation means developing alternative strategies to accomplish tasks despite persistent impairments, such as using your unaffected hand for activities previously done with the affected hand. Both contribute to improved independence and quality of life.
How long can meaningful recovery continue after a stroke?
Neuroplasticity continues throughout life, allowing recovery years after stroke with appropriate intensive therapy. While the most rapid gains typically occur in the first three to six months, research demonstrates that customized high-intensity rehabilitation produces meaningful improvements even in chronic stroke survivors. Continued practice maintains and builds upon earlier gains.
How can caregivers manage stress while supporting stroke recovery?
Caregivers should establish clear boundaries, join support groups, communicate openly with healthcare providers, prioritize their own health, and accept help from others. Respite care services provide temporary relief, while counseling addresses emotional challenges. Recognizing that caregiver wellbeing directly impacts patient outcomes justifies investing time and resources in self-care.
Does technology replace human expertise in neurorehabilitation?
No, technology enhances therapy delivery but does not replace skilled clinicians who assess individual needs, adjust interventions, and provide essential human connection. Advanced devices like robot-assisted therapy and adaptive stimulation systems optimize practice intensity and precision, but successful outcomes depend on expert guidance in selecting appropriate tools, customizing protocols, and integrating technology within comprehensive rehabilitation programs.
Can home-based rehabilitation produce results comparable to clinic-based therapy?
Yes, when properly designed and implemented with adequate intensity and frequency. Home rehabilitation allows greater total practice volume, immediate application to real-world tasks, and reduced barriers to consistent participation. Combining periodic clinical supervision with daily home practice often produces superior outcomes compared to clinic-only therapy with limited frequency.
Recommended
38
Get inspired by a stroke recovery story
Home rehabilitation at full speed.
My husband suffered a severe stroke on August 19, 2020, which paralyzed him on the right side. Thanks to FitMi he has made huge progress since then. He still has no strength in his right arm, but now he can walk with a cane, his speech has improved significantly, and he is fighting and rehabilitating at full speed. We are very happy that we bought this FitMi kit for him, so he can continue his training and exercises at home. We are encouraged by this program and the positive reviews we read from others who used it. Thank God we found this kit and thank you for your support. It is a wonderful program.
Kate (08.09.2020)








