Post-stroke therapy explained: effective recovery methods 2026
Stroke recovery doesn’t follow a one-size-fits-all pattern, despite common beliefs about predictable outcomes. Many survivors and caregivers face confusion when recovery timelines and results vary widely from person to person. Recent research challenges long-held assumptions about fixed recovery proportions, revealing that individualized therapy approaches matter more than ever. This guide explains proven post-stroke therapy methods, optimal timing for rehabilitation, and practical tools that support motor function recovery at home and in clinical settings, helping you make informed decisions for your recovery journey.
Table of Contents
- The Importance Of Early Post-Stroke Rehabilitation
- How Physical Therapy Supports Motor Recovery After Stroke
- Understanding Recovery Variability And The Proportional Recovery Rule
- Applying Effective Therapy Tools At Home And In Clinics
- Explore Targeted Post-Stroke Rehabilitation Kits
- Frequently Asked Questions
Key takeaways
| Point | Details |
|---|---|
| Early rehab timing | Starting therapy within 24 to 48 hours after stroke is safe and prevents complications from bed rest. |
| Physical therapy benefits | Targeted exercises improve strength, coordination, and balance, forming the foundation for motor recovery. |
| Recovery variability | Fixed proportional recovery claims face scientific critique; individual trajectories differ significantly. |
| Home therapy value | Consistent use of rehab tools at home complements clinical therapy and boosts recovery outcomes. |
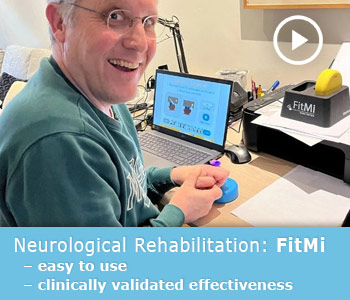
| Targeted devices | Specialized kits like FitMi and MusicGlove enable engaging, trackable motor function exercises. |
 The importance of early post-stroke rehabilitation
The importance of early post-stroke rehabilitation
Starting rehabilitation immediately after a stroke makes a critical difference in your recovery trajectory. Early rehabilitation within 24 to 48 hours of acute stroke onset is safe and helps minimize complications that arise from prolonged bed rest. When you remain immobile, your muscles weaken rapidly, your cardiovascular system deconditions, and you face increased risks of pneumonia, pressure sores, and blood clots.
Early therapy counteracts these dangers by maintaining muscle strength and joint mobility from the start. Your medical team can safely initiate gentle exercises even while you’re in acute care, tailoring activities to your specific condition and abilities. This early intervention doesn’t just prevent secondary complications; it jumpstarts both physical and neurological recovery processes that are crucial for regaining function.
The benefits of timely rehabilitation extend beyond the hospital. Early therapy establishes momentum that carries into your transition home, where continuing exercises becomes part of your daily routine. Understanding the role of home rehabilitation helps you maintain progress between clinical sessions.
Pro Tip: Ask your medical team about starting simple exercises like ankle pumps, gentle arm movements, or seated balance activities within the first two days after your stroke, even if you’re still in the hospital.
Key early rehabilitation activities include:
- Passive range of motion exercises to prevent joint stiffness
- Gentle muscle activation to maintain strength
- Seated balance training to prepare for standing
- Breathing exercises to prevent respiratory complications
- Swallowing assessments and exercises when needed
“The sooner you begin rehabilitation, the better your chances of regaining lost abilities and independence. Early therapy sets the foundation for everything that follows in your recovery journey.”
How physical therapy supports motor recovery after stroke
Physical therapy forms the cornerstone of stroke rehabilitation by systematically addressing the motor impairments that affect your daily life. Physical therapy helps stroke patients improve their strength, coordination, and balance, creating the foundation you need to regain independence in walking, transferring, and performing everyday activities.
Your physical therapist designs exercises targeting specific muscle groups weakened by the stroke. These exercises progress gradually from simple movements to complex functional tasks. You might start with assisted leg lifts in bed and advance to walking with support, then to navigating stairs independently. Each step builds on previous gains, reinforcing neural pathways that control movement.
Coordination exercises help your brain relearn how to control multiple muscle groups simultaneously. Activities like reaching for objects at different heights, stepping over obstacles, or practicing weight shifts challenge your neuromuscular system to work efficiently. This repetitive practice strengthens the communication between your brain and muscles.
Balance training reduces fall risk while improving your confidence in moving safely. Your therapist might use balance boards, foam pads, or simple standing exercises to challenge your stability systems. Better balance translates directly to safer mobility at home and in your community.

Physical therapy rarely works in isolation. Your care team typically includes occupational therapists who focus on arm and hand function, speech therapists addressing swallowing and communication, and sometimes recreational therapists. This interdisciplinary approach ensures all aspects of your recovery receive attention. Exploring motor rehab improving movement provides deeper insights into these integrated approaches.
Effective physical therapy follows these principles:
- Assessment of your specific impairments and functional limitations
- Goal setting based on activities meaningful to your daily life
- Progressive exercise programs that challenge without overwhelming
- Frequent repetition to strengthen motor learning
- Regular reassessment and program adjustments as you improve
- Education for you and your caregivers about home exercises
Consistency matters more than intensity in many cases. Regular, focused practice yields better results than sporadic intensive sessions. Your therapist will recommend a schedule that balances therapeutic benefit with rest and recovery time.
Pro Tip: Keep a simple log of your exercises and any improvements you notice, no matter how small. Tracking progress helps you stay motivated and provides valuable information for your therapy team.
Many survivors benefit from learning the best rehabilitation exercises after stroke to supplement their formal therapy sessions with effective home practice.
Understanding recovery variability and the proportional recovery rule
Stroke recovery patterns vary dramatically among individuals, challenging the notion that everyone follows a predictable path. For years, the proportional recovery rule suggested that most survivors recover approximately 70% of their lost function, but this concept faces significant scientific scrutiny today.
The proportional recovery rule emerged from observations that patients with moderate initial impairments seemed to regain a consistent proportion of function. However, the proportional recovery rule is critiqued due to confounded correlation of initial scores with change over time. This statistical flaw means the apparent pattern might reflect mathematical artifacts rather than biological reality.
Recent research has prompted a fundamental reassessment of how we understand recovery trajectories. Two prominent papers reassessed patients’ behavioral trajectory following stroke, revealing that recovery patterns are far more individualized than previously thought. These studies highlight that factors like stroke location, size, your age, pre-stroke fitness, therapy intensity, and motivation all interact to shape your unique recovery path.
Some survivors experience rapid initial gains that plateau within weeks, while others show steady improvement over months or years. A few individuals who start with severe impairments make remarkable recoveries that defy statistical predictions, while others with seemingly minor strokes struggle with persistent deficits. This variability underscores why personalized therapy plans matter more than generic protocols.
| Recovery Factor | Impact on Outcomes | Clinical Implication |
|---|---|---|
| Stroke severity | Larger strokes typically cause greater initial impairment | Baseline assessment guides realistic goal setting |
| Lesion location | Motor cortex damage affects movement differently than other areas | Imaging helps predict specific deficits |
| Therapy intensity | Higher repetition counts improve motor learning | Consistent practice accelerates gains |
| Time since stroke | Neuroplasticity is highest early but continues long term | Never assume recovery window has closed |
| Individual factors | Age, fitness, motivation, and support systems vary widely | Personalized approaches outperform standardized programs |
Understanding neuroplasticity and stroke recovery helps explain why your brain retains the capacity to reorganize and form new neural connections throughout your recovery journey. This biological flexibility means that improvement remains possible even when statistical models might suggest otherwise.
Recognizing the signs of recovery after stroke helps you and your caregivers identify progress, whether it follows expected patterns or takes a unique trajectory.
Key factors influencing your recovery path:
- Stroke type, location, and extent of brain tissue damage
- Your age, overall health, and pre-stroke functional level
- Speed and quality of acute medical treatment received
- Intensity, frequency, and duration of rehabilitation therapy
- Presence of complications like infections or additional strokes
- Emotional and psychological factors including depression and motivation
- Quality of social support and home environment
“Your recovery is uniquely yours. While research provides general guidance, your individual journey depends on multiple interacting factors that make predictions uncertain. Focus on consistent effort rather than comparing yourself to statistical averages.”
Pro Tip: Avoid comparing your recovery timeline to others, even those with seemingly similar strokes. Your unique combination of factors means your path will differ, and progress might appear in unexpected ways.
 Applying effective therapy tools at home and in clinics
Applying effective therapy tools at home and in clinics
Modern rehabilitation technology brings clinical-quality therapy into your home, complementing traditional physical therapy sessions. Specialized therapy kits and devices enable you to practice targeted exercises that improve motor skills through engaging, repetitive activities that your brain needs for recovery.
These tools work by providing structured, trackable exercises that target specific motor functions. The FitMi system, for example, guides you through interactive exercises that challenge both gross and fine motor skills, automatically adjusting difficulty as you improve. The MusicGlove rehabilitation device uses music-based hand exercises that make repetitive finger movements engaging rather than tedious.
Home therapy devices offer several advantages over relying solely on clinic visits. You can practice multiple times daily at your convenience, accumulating the high repetition counts that drive motor learning. Many devices track your performance, showing progress that might be too gradual to notice day to day. This feedback motivates continued effort and provides objective data for your therapy team.
Clinical settings often integrate advanced devices that therapists operate, combining technology with professional guidance. These might include robotic assist devices, virtual reality systems, or biofeedback equipment that provides real-time information about muscle activation. Your therapist uses these tools to challenge you appropriately while ensuring safety and proper technique.
The most effective approach combines home tools with professional therapy. Your physical therapist assesses your needs, recommends appropriate devices, and teaches you proper use. You practice at home between sessions, and your therapist monitors progress, adjusting your program as needed. This partnership maximizes the benefits of both approaches.
Benefits of home rehabilitation tools:
- Enable consistent daily practice without travel to clinics
- Provide immediate feedback on performance and progress
- Make repetitive exercises engaging through games and music
- Allow family members to participate in your therapy
- Reduce costs compared to frequent professional sessions
- Build confidence through independent practice
| Tool Type | Primary Focus | Best For | Typical Use |
|---|---|---|---|
| FitMi system | Full body motor skills | Arm, hand, leg, core exercises | 20-30 minutes daily at home |
| MusicGlove | Hand and finger function | Fine motor skills, grip strength | 30-60 minutes several times weekly |
| Balance boards | Stability and core strength | Fall prevention, standing balance | 10-15 minutes with supervision |
| Resistance bands | Muscle strengthening | Targeted muscle groups | During therapy sessions and at home |
| Therapy balls | Coordination and grip | Hand function, core stability | Integrated into exercise routines |
Exploring available rehabilitation aids helps you identify tools suited to your specific needs and recovery goals. The home neurorehab system offers comprehensive motor training, while the hand and finger rehab glove targets upper extremity recovery specifically.
Pro Tip: Start with shorter practice sessions and gradually increase duration as your endurance improves. Quality of movement matters more than quantity, so focus on performing exercises correctly rather than rushing through repetitions.
Research confirms that physical therapy improves strength, coordination, and balance, and home tools extend these benefits by enabling the frequent practice necessary for optimal motor recovery.
Explore targeted post-stroke rehabilitation kits
Tisele Rehab specializes in innovative rehabilitation solutions designed specifically for stroke survivors and individuals with neurological conditions. Our product line focuses on evidence-based tools that bring clinical-quality therapy into your home, supporting your recovery journey with engaging, effective exercises.
The FitMi home neurorehab system delivers comprehensive motor training through interactive exercises that adapt to your ability level. The MusicGlove rehab glove transforms hand therapy into an engaging musical experience, making the repetitive practice essential for recovery feel less like work. Both products integrate seamlessly with professional therapy programs, extending your progress between clinical sessions. Explore Tisele Rehab rehabilitation kits to find solutions that match your specific recovery needs and goals.
Frequently asked questions
What is the best time to start post-stroke therapy?
Starting rehabilitation within 24 to 48 hours after stroke onset is safe and beneficial for most patients. Early therapy prevents complications from bed rest and initiates motor recovery sooner. Your medical team will assess your specific condition to determine the appropriate timing and intensity for beginning exercises.
How does physical therapy improve stroke recovery?
Physical therapy strengthens muscles, improves coordination, and enhances balance after stroke. Therapists design progressive exercise programs that challenge your motor systems, promoting neuroplasticity and functional improvements. Consistent practice of targeted exercises helps your brain relearn movement patterns, supporting motor rehab improving movement throughout your recovery.
Are home rehabilitation tools effective for stroke recovery?
Yes, home therapy devices support consistent practice between professional sessions, which is crucial for motor learning. Tools like FitMi and MusicGlove provide structured, engaging exercises that complement clinical therapy. Understanding the role of home rehabilitation shows how regular home practice accelerates progress and maintains gains achieved during formal therapy sessions.
Does everyone recover the same percentage of function after stroke?
No, recovery varies significantly among individuals based on stroke severity, location, therapy intensity, and personal factors. The proportional recovery rule suggesting fixed recovery percentages faces scientific critique due to statistical flaws. Your unique combination of factors determines your recovery trajectory, making personalized therapy approaches more effective than standardized protocols.
How long does stroke recovery take?
Recovery timelines vary widely, with most rapid gains occurring in the first three to six months. However, improvements can continue for years with consistent therapy. Neuroplasticity allows your brain to reorganize and form new connections long after the initial stroke, meaning the recovery window never truly closes for motivated individuals who continue therapeutic activities.
Recommended
- Neuroplasticity: Driving Faster Stroke Recovery Outcomes
- TiSale Rehab Ltd.
- Rehabilitation Workflow for Patients: Effective Therapy Guide
- BETTER REHAB STARTS HERE !
- PTSD Treatment Duration: Complete Guide for Recovery | Glendora Recovery Center
- How voice therapy works: natural recovery for pros 2026 - TMRG Solutions
38
Get inspired by a stroke recovery story
Home rehabilitation at full speed.
My husband suffered a severe stroke on August 19, 2020, which paralyzed him on the right side. Thanks to FitMi he has made huge progress since then. He still has no strength in his right arm, but now he can walk with a cane, his speech has improved significantly, and he is fighting and rehabilitating at full speed. We are very happy that we bought this FitMi kit for him, so he can continue his training and exercises at home. We are encouraged by this program and the positive reviews we read from others who used it. Thank God we found this kit and thank you for your support. It is a wonderful program.
Kate (08.09.2020)








