Top stroke recovery strategies 2026 for lasting results
Stroke survivors and caregivers face overwhelming choices when selecting rehabilitation approaches in 2026. With innovative technologies like brain-computer interfaces, robotic systems, and adaptive neurofeedback now entering clinical practice, understanding which strategies deliver genuine results becomes critical. This guide examines evidence-based methods proven to enhance motor function and daily living, helping you navigate the most effective options for meaningful recovery.
Table of Contents
- Criteria For Selecting Effective Stroke Recovery Strategies In 2026
- Brain-Computer Interface (Bci) Technologies In Stroke Rehabilitation
- Robotic-Assisted Therapy And Myoelectric Control For Upper Limb Recovery
- Comparing Top Stroke Recovery Strategies: Brain-Computer Interfaces, Robotics, And Neurofeedback
- Explore Effective Stroke Rehabilitation Kits And Tools
- What Are The Most Effective Stroke Recovery Strategies In 2026?
Key takeaways
| Point | Details |
|---|---|
| Early intervention matters | Therapies started in acute or subacute phases with over 12 hours total dose show superior outcomes compared to delayed treatment. |
| BCI technology advances recovery | Brain-computer interfaces help reconstruct neural pathways and improve motor function and daily activities in both acute and chronic stroke patients. |
| Robotic systems enhance function | Robotic-assisted therapy significantly improves motor function, grip strength, and social participation when combined with conventional rehabilitation. |
| Adaptive feedback optimizes training | Myoelectric control with VR feedback helps normalize muscle activation patterns and accelerates upper limb recovery in stroke survivors. |
 Criteria for selecting effective stroke recovery strategies in 2026
Criteria for selecting effective stroke recovery strategies in 2026
Choosing the right rehabilitation approach requires understanding what separates effective interventions from less impactful ones. Evidence now clearly shows that timing and dose both influence recovery success, with interventions started early and delivered intensively producing better outcomes.
When evaluating recovery strategies, consider these key factors:
- Timing of intervention: Starting therapy during acute or subacute phases typically yields superior results compared to delayed treatment.
- Total therapy dose: Research indicates that exceeding 12 hours of total therapy dose correlates with meaningful functional gains.
- Intensity and duration: Higher intensity sessions over adequate timeframes drive neuroplastic changes more effectively than sporadic efforts.
- Individual impairment profile: Match intervention complexity and type to your specific motor deficits and recovery stage.
- Technology integration: Combine emerging tools with conventional rehabilitation for comprehensive, multimodal recovery.
Your recovery stage matters significantly. Acute phase patients may benefit from intensive conventional therapy combined with technological augmentation. Chronic stroke survivors often see gains from neurofeedback and BCI approaches that target persistent impairments. Understanding where you fall on this timeline helps prioritize interventions appropriately.
Pro Tip: Track your therapy hours weekly to ensure you meet the evidence-based threshold of 12+ hours total dose during critical early recovery windows. Small daily sessions accumulate faster than you think.
The 7 essential rehab tips framework provides additional guidance on structuring your rehabilitation program for maximum effectiveness.
Brain-computer interface (BCI) technologies in stroke rehabilitation
Brain-computer interfaces represent a breakthrough in helping stroke survivors regain motor control by directly translating brain signals into movement commands. These systems work by detecting neural activity associated with movement intention, then providing real-time feedback that helps reconstruct damaged neural pathways.
Clinical evidence demonstrates that BCI interventions benefit lower limb motor function and activities of daily living in stroke patients across different recovery phases. The technology proves particularly valuable because it engages your brain’s natural learning mechanisms, strengthening the connection between intention and action.
Motor imagery combined with BCI (MI-BCI) shows especially promising results. When you use MI-BCI as adjunct therapy, you enhance both motor function scores and daily living capabilities compared to conventional rehabilitation alone. This approach works by having you mentally rehearse movements while the BCI system provides feedback confirming when your brain generates appropriate motor signals.
“Noninvasive closed-loop neurofeedback can guide motor recovery in post-stroke patients with chronic motor impairment, yielding clinically significant improvements.”
Key advantages of BCI technology include:
- Chronic phase effectiveness: Works even years after stroke when traditional therapy plateaus.
- Neural pathway reconstruction: Actively rebuilds damaged motor control circuits through targeted feedback.
- Personalized intensity: Adapts difficulty to your current capability level automatically.
- Engagement enhancement: Provides immediate visual or sensory confirmation of neural activity.
The noninvasive nature of modern BCI systems makes them practical for both clinical and home settings. Closed-loop neurofeedback yields measurable motor improvement without surgery or implanted devices, reducing barriers to access.
While evidence remains promising, current BCI research involves relatively small sample sizes. Larger trials underway in 2026 aim to establish definitive protocols and identify which patient profiles benefit most. For now, combining BCI with motor rehab improvements and best rehab exercises after stroke provides the most comprehensive approach.
Consider exploring stroke rehabilitation BCI meta-analysis research for deeper technical understanding of mechanisms and outcomes.
Robotic-assisted therapy and myoelectric control for upper limb recovery
Robotic exoskeleton systems transform upper limb rehabilitation by providing precisely controlled, repeatable movement assistance that intensifies therapy beyond what manual techniques achieve alone. These devices support your affected arm through functional movement patterns while measuring performance metrics in real time.
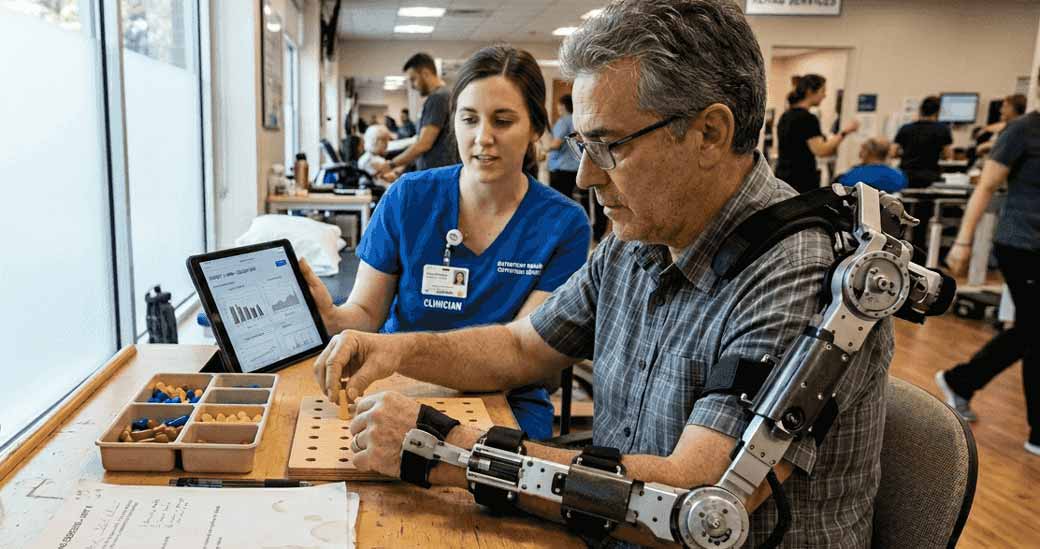
The ReHand robotic system demonstrates how effectively these technologies work. Studies show ReHand robot enhances upper limb recovery in subacute stroke patients when added to standard therapy protocols. The portable design allows intensive practice sessions that would exhaust a human therapist, delivering higher repetition counts critical for motor learning.
Myoelectric control adds another powerful dimension to robotic therapy. This approach captures residual electrical signals from your muscles, even weak ones, and translates them into movement commands for assistive devices or virtual avatars. When combined with adaptive visual feedback in VR environments, myoelectric control with VR feedback improves muscle activation patterns and movement quality.
The adaptive feedback component proves particularly valuable because it automatically adjusts visual gain based on your performance. If you generate weak signals, the system amplifies the visual response to maintain motivation and engagement. As your control improves, feedback scaling changes to challenge you appropriately.
Comparison of robotic therapy approaches
| System Type | Primary Mechanism | Best For | Key Advantage |
|---|---|---|---|
| Exoskeleton robots | Physical movement assistance | Severe impairment, subacute phase | High repetition count, objective metrics |
| Myoelectric control | Residual signal amplification | Moderate impairment, chronic phase | Engages remaining neural pathways |
| VR-integrated systems | Adaptive visual feedback | All severity levels | Increases motivation and engagement |
| End-effector robots | Task-oriented training | Functional goal practice | Translates directly to daily activities |
Meta-analyses confirm that robotic-assisted therapy significantly improves multiple outcome domains including motor function, grip strength, activities of daily living, and social participation. These comprehensive benefits justify the equipment investment for many rehabilitation programs.
Pro Tip: When using robotic systems, focus on quality of movement intention rather than just completing repetitions. The neuroplastic benefits come from actively engaging your brain in the movement, not passively allowing the robot to move your arm.
Integrating robotic therapy with conventional exercises maximizes outcomes. While robots excel at repetitive practice and objective measurement, they complement rather than replace hands-on therapy, functional training, and home rehabilitation in stroke recovery programs.
The technology in neuro recovery landscape continues evolving rapidly, with 2026 bringing more affordable, portable options suitable for home use alongside clinical-grade systems.
Explore detailed protocols in the ReHand robotic system trial to understand how these interventions integrate into comprehensive rehabilitation programs.
Comparing top stroke recovery strategies: brain-computer interfaces, robotics, and neurofeedback
Understanding how leading rehabilitation technologies compare helps you make informed decisions about which approaches suit your specific recovery needs and circumstances. Each method targets different aspects of motor recovery through distinct mechanisms.
Strategy comparison matrix
| Strategy | Therapeutic Target | Primary Advantages | Limitations | Evidence Quality |
|---|---|---|---|---|
| BCI systems | Neural pathway reconstruction | Effective in chronic phase, noninvasive | Variable results, small sample studies | Moderate, improving |
| Robotic therapy | Physical movement training | High repetition, objective data, proven efficacy | Equipment access, cost | Strong, meta-analyses available |
| Adaptive neurofeedback | Brain activity modulation | Personalized difficulty, real-time feedback | Emerging technology, limited long-term data | Promising, needs larger trials |
| Myoelectric control | Residual signal amplification | Uses existing neural capacity, motivating | Requires some muscle activity | Moderate, growing evidence |
 Comprehensive review of BCI rehabilitation methods highlights that while each approach shows promise, significant evidence gaps remain regarding optimal protocols, patient selection criteria, and home/community implementation.
Comprehensive review of BCI rehabilitation methods highlights that while each approach shows promise, significant evidence gaps remain regarding optimal protocols, patient selection criteria, and home/community implementation.
BCI technology excels when conventional therapy reaches a plateau, particularly in chronic stroke survivors. The ability to work directly with neural signals rather than requiring physical movement makes it valuable for severe impairments. However, response variability between individuals means some patients benefit dramatically while others see modest gains.
Robotic-assisted therapy currently offers the strongest evidence base across multiple outcome measures. The technology particularly benefits subacute patients and those with severe impairments who need intensive, repetitive practice. Access remains a barrier since many systems require clinical settings, though portable options emerging in 2026 address this limitation.
Adaptive neurofeedback approaches like the Magnetic NeuroRing represent exciting frontiers in rehabilitation technology. These systems modulate brain activity patterns in real time, potentially accelerating motor learning. Early results show promise but larger validation studies continue throughout 2026.
Combining multiple approaches often yields superior outcomes compared to single-method protocols. For example, pairing BCI feedback with robotic assistance leverages both neural training and physical practice benefits. Similarly, conventional therapy provides the functional context that makes technological interventions translate into real-world capability.
Research gaps you should know about include limited data on long-term outcomes beyond initial intervention periods, small sample sizes in many studies, and insufficient investigation of which patient characteristics predict best response to specific technologies. The neuroplasticity in stroke recovery principles underlying these methods are well-established, but optimal application protocols continue evolving.
When selecting strategies, prioritize evidence-based approaches appropriate for your recovery phase and impairment severity. Early-phase survivors typically benefit most from intensive conventional therapy augmented selectively with technology. Chronic-phase individuals often find greater value in BCI and neurofeedback approaches that target persistent deficits resistant to traditional methods.
Review the BCI strategies review for technical details on implementation considerations and outcome measurement approaches across different technology categories.
Explore effective stroke rehabilitation kits and tools
Translating research insights into practical recovery requires accessible tools that bring evidence-based therapy into your daily routine. Rehabilitation technology no longer requires clinical settings exclusively, with sophisticated home-based systems now delivering professional-grade interventions.
Tisele Rehab offers rehabilitation kits for stroke recovery designed around the same neuroplastic principles driving clinical technologies. Products like the FitMi home neurorehabilitation system provide interactive, game-based exercises that increase therapy dose between formal sessions. The MusicGlove hand rehabilitation device uses engaging activities to deliver the repetitive practice essential for motor learning, making it easier to achieve the 12+ hour therapy threshold associated with better outcomes. These tools complement advanced strategies like BCI and robotic therapy by ensuring consistent progress throughout your recovery journey, not just during scheduled appointments.
What are the most effective stroke recovery strategies in 2026?
What stroke recovery strategies show the strongest evidence in 2026?
Brain-computer interfaces, robotic-assisted therapy, and adaptive neurofeedback demonstrate significant benefits across multiple clinical trials. Conventional therapy remains foundational, with technology augmenting rather than replacing traditional approaches for optimal outcomes.
How soon should I start intensive stroke rehabilitation?
Begin as early as medically safe, ideally during acute or subacute phases. Early intervention with adequate dose (over 12 hours total) consistently produces superior functional gains compared to delayed treatment.
Can chronic stroke survivors benefit from new rehabilitation technologies?
Absolutely. BCI systems and adaptive neurofeedback show particular promise for chronic-phase recovery when traditional therapy plateaus. These technologies engage neural plasticity mechanisms that remain active years after stroke.
Do I need clinical settings for effective stroke rehabilitation?
While clinical programs provide important structure and expertise, home-based therapy tools significantly increase total practice time. Combining professional sessions with consistent home practice using evidence-based systems maximizes recovery potential.
How do robotic systems improve stroke recovery outcomes?
Robotic therapy delivers high-repetition practice with precise movement assistance and objective performance tracking. Studies confirm improvements in motor function, grip strength, daily activities, and social participation when added to standard rehabilitation.
What role does therapy dose play in stroke recovery?
Therapy dose directly impacts outcomes, with research showing 12+ total hours as a meaningful threshold. Higher intensity and duration drive stronger neuroplastic changes, making consistent daily practice essential for meaningful functional gains.
Recommended
38
Get inspired by a stroke survival story
It's a very good "gaming" therapy.
I had a stroke 9 years ago and have tried many different therapies. I really like the gaming aspect offered by MusicGlove. I have only been using this kit for a month and I can already see some progress. It helps me a lot to stay motivated. It's really amazing...
In summary, I really like MusicGlove. MusicGlove.
Tomasz S. (04.03.2020)









