What is motor recovery? A guide for stroke and neuro rehab
Motor recovery after stroke or neurological injury often feels like navigating uncharted territory. Many survivors and caregivers struggle to understand what motor recovery truly means, why certain therapies work, and how to maximize rehabilitation outcomes. This confusion can delay progress and diminish hope during a critical healing window. Understanding the science behind motor recovery, the role of neuroplasticity, and practical rehabilitation strategies empowers you to take an active role in recovery. This guide breaks down motor recovery fundamentals, compares rehabilitation approaches, and introduces effective tools and exercises that accelerate functional restoration for stroke survivors and individuals with neurological conditions.
Table of Contents
- Understanding Motor Recovery: What It Means And Why It Matters
- Key Mechanisms Driving Motor Recovery: Neuroplasticity And Rehabilitation
- Comparing Rehabilitation Approaches: Home Rehab Vs. Clinical Therapy
- Effective Rehabilitation Tools And Exercises For Motor Recovery
- Explore Rehabilitation Kits And Aids For Motor Recovery
- Frequently Asked Questions
Key takeaways
| Point | Details |
|---|---|
| Motor recovery restores movement | Regaining coordination and motor function after neurological injury through targeted rehabilitation |
| Neuroplasticity powers healing | The brain rewires itself to compensate for damaged areas and support movement restoration |
| Consistent therapy drives results | Regular, challenging exercises stimulate brain changes that improve motor outcomes |
| Multiple rehab settings work | Combining home practice with clinical therapy maximizes recovery potential |
| Early intervention matters most | Starting rehabilitation quickly after injury leads to significantly better functional gains |
 Understanding motor recovery: What it means and why it matters
Understanding motor recovery: What it means and why it matters
Motor recovery represents the process of regaining movement, coordination, and functional motor skills after neurological injury such as stroke, traumatic brain injury, or cerebral palsy. Unlike simple healing, motor recovery is a complex process involving neural plasticity and relearning motor skills that requires active participation rather than passive rest. The brain must reorganize neural pathways to compensate for damaged areas, essentially teaching undamaged regions to take over lost functions.
Neuroplasticity serves as the foundation for this recovery. When stroke damages brain tissue controlling specific movements, surrounding healthy neurons can form new connections to restore those functions. This rewiring happens most effectively when you actively practice movements repeatedly, creating the neural demand that triggers brain reorganization. Think of it like building a detour when a highway closes: the brain creates alternative routes to reach the same destination.
Motor recovery addresses several interconnected challenges:
- Muscle weakness or paralysis affecting one or both sides of the body
- Spasticity causing involuntary muscle contractions and stiffness
- Impaired coordination making smooth, controlled movements difficult
- Loss of fine motor skills needed for daily tasks like buttoning clothes or writing
- Balance and gait problems affecting walking safety and independence
Early and consistent rehabilitation interventions significantly impact recovery outcomes. The first three to six months after injury represent a critical window when the brain shows heightened plasticity and responds most dramatically to therapy. However, recovery continues beyond this period with dedicated practice.
Pro Tip: Active participation in exercises produces better results than passive therapies alone because movement practice creates the neural stimulation needed to drive brain rewiring and functional improvements.
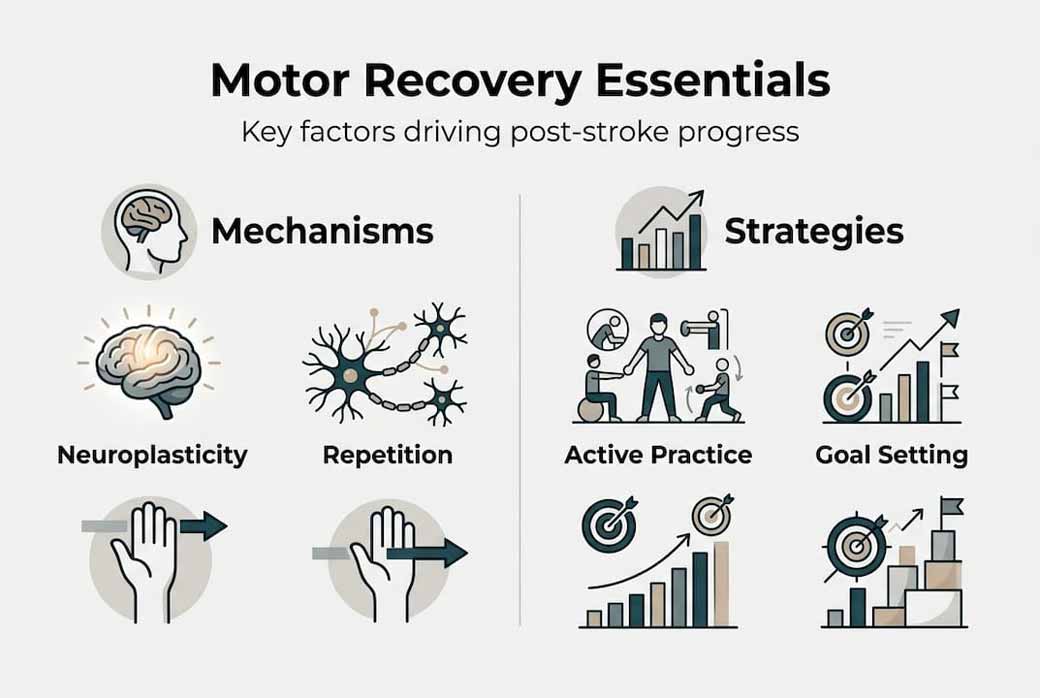
Key mechanisms driving motor recovery: neuroplasticity and rehabilitation
Neuroplasticity enables the brain to reorganize itself, which is essential for regaining motor function after stroke or neurological damage. This adaptive capacity allows healthy brain regions to assume control over movements previously managed by damaged areas. The process involves forming new neural connections, strengthening existing pathways, and sometimes recruiting entirely different brain regions to support motor tasks.
Rehabilitation exercises stimulate neuroplastic changes through repetitive, purposeful movement practice. When you perform a specific motion repeatedly, you send consistent signals to the brain that this movement matters. The brain responds by allocating more neural resources to that task, strengthening the connections involved, and improving efficiency. This explains why stroke survivors who practice reaching movements hundreds of times daily show measurably better arm function than those practicing less frequently.
Common therapeutic techniques harness neuroplasticity through several evidence-based approaches:
- Task-specific training focusing on movements needed for daily activities
- Constraint-induced movement therapy forcing use of affected limbs
- Repetitive practice performing the same motion many times per session
- Progressive difficulty gradually increasing task complexity as skills improve
- Biofeedback providing real-time information about movement quality
Consistency and challenge in therapy enhance brain rewiring more effectively than sporadic or easy exercises. Your brain adapts most when pushed slightly beyond current capabilities, a concept called progressive overload. Performing 10 challenging repetitions creates more neuroplastic change than 100 easy ones. Similarly, daily 30-minute sessions produce better outcomes than weekly two-hour sessions because regular practice maintains the neural stimulation needed for lasting changes.
The relationship between neuroplasticity and stroke recovery demonstrates why passive treatments like massage provide temporary relief but active exercise creates permanent improvement. Movement practice literally reshapes your brain’s structure and function.
Pro Tip: Incorporating variety in rehabilitation tasks prevents plateauing by challenging the brain in different ways, maintaining engagement, and promoting broader functional improvements rather than narrow skill development.
Comparing rehabilitation approaches: home rehab vs. clinical therapy
Clinical therapy involves working with licensed therapists in hospital, outpatient, or specialized rehabilitation facilities. These settings provide professional guidance, access to specialized equipment like robotic devices or virtual reality systems, and structured programs tailored to individual needs. Therapists assess progress, adjust treatment plans, and ensure proper technique to prevent compensatory movement patterns that could hinder recovery. The supervised environment also offers safety for patients with severe impairments who need assistance during exercises.

Home rehabilitation offers distinct advantages that complement clinical care. Convenience allows more frequent practice sessions since you eliminate travel time and scheduling constraints. This increased practice volume directly translates to better outcomes because neuroplasticity responds to repetition. Home rehab also empowers patients to take ownership of recovery, building confidence and self-efficacy that enhance motivation. Cost represents another factor, as home exercises require minimal expense compared to ongoing clinical sessions.
Challenges exist in both settings. Clinical therapy costs add up quickly, and insurance often limits covered sessions. Home rehab requires self-discipline to maintain consistent practice without external accountability. Equipment availability varies, though many effective exercises need only simple household items. Supervision level differs dramatically: clinical settings provide expert oversight while home practice relies on patient judgment and occasional caregiver assistance.
| Aspect | Clinical Therapy | Home Rehabilitation |
|---|---|---|
| Setting | Hospital or outpatient facility | Patient’s residence |
| Supervision | Licensed therapist present | Self-directed or caregiver assisted |
| Cost | High, insurance dependent | Low, minimal equipment needed |
| Accessibility | Limited by appointments | Available anytime |
| Equipment | Specialized devices | Basic tools or household items |
| Frequency | 1 to 3 sessions weekly | Daily practice possible |
| Personalization | Expert-tailored programs | Patient-adapted exercises |
Best practices maximize results regardless of setting:
- Maintain consistent daily practice schedules rather than sporadic intensive sessions
- Focus on quality repetitions with proper form over quantity with poor technique
- Track progress using measurable metrics like range of motion or task completion time
- Communicate regularly between home practice and clinical team for coordinated care
- Combine both approaches when possible for professional guidance plus frequent home practice
Optimal motor recovery typically involves integrating clinical expertise with home practice volume. Therapists design programs and monitor progress while patients implement daily exercises, creating a partnership that leverages both professional knowledge and neuroplastic benefits of frequent repetition.
Effective rehabilitation tools and exercises for motor recovery
Rehabilitation tools designed for neurological recovery provide structured, engaging ways to practice movements repeatedly. FitMi rehabilitation kits use interactive gaming elements to motivate hundreds of repetitions per session, targeting both upper and lower body motor functions. The system adapts difficulty automatically as skills improve, maintaining the optimal challenge level for neuroplastic gains. MusicGlove focuses specifically on hand and finger recovery through music-based exercises that make repetitive practice enjoyable rather than tedious.
| Tool | Target Function | Key Benefits |
|---|---|---|
| FitMi | Full body motor skills | Interactive gaming, automatic progression, bilateral training |
| MusicGlove | Hand and finger dexterity | Music-based motivation, grip strength, fine motor precision |
| Therapy putty | Hand strength | Variable resistance, portable, affordable |
| Balance boards | Standing stability | Core engagement, fall prevention, proprioception |
| Resistance bands | Limb strengthening | Adjustable difficulty, multiple exercise options |
Top rehabilitation exercises for motor recovery include:
- Reach and grasp practice: Place objects at various heights and distances, practicing controlled reaching and grasping movements 20 to 30 times per session to improve arm coordination and hand function.
- Sit to stand transfers: Practice standing from a chair without using hands if possible, focusing on weight shifting and leg strengthening through 10 to 15 repetitions multiple times daily.
- Finger isolation exercises: Touch each fingertip to thumb sequentially, then reverse the pattern, performing 3 sets of 10 repetitions to enhance fine motor control.
- Ankle pumps and circles: While seated or lying down, move ankles up and down then in circles, completing 20 repetitions each direction to maintain ankle mobility and prevent stiffness.
- Weight shifting practice: While standing with support, shift weight from one leg to the other, holding each position for 5 seconds and repeating 15 times to improve balance and prepare for walking.
- Pinch strengthening: Use clothespins or therapy putty to practice pinching motions, completing 20 to 30 repetitions to build hand strength needed for daily tasks.
- Step practice: Step up onto a low platform or stair with the affected leg, then step down, performing 10 to 15 repetitions to build leg strength and coordination.
 Repetition, intensity, and motivation determine exercise effectiveness more than equipment sophistication. Performing movements hundreds of times creates the neural stimulation needed for brain rewiring. Intensity means working at a challenging but achievable level, not coasting through easy motions. Motivation sustains the consistent practice required for meaningful recovery, which is why engaging tools and varied exercises help maintain long-term adherence.
Repetition, intensity, and motivation determine exercise effectiveness more than equipment sophistication. Performing movements hundreds of times creates the neural stimulation needed for brain rewiring. Intensity means working at a challenging but achievable level, not coasting through easy motions. Motivation sustains the consistent practice required for meaningful recovery, which is why engaging tools and varied exercises help maintain long-term adherence.
Pro Tip: Set measurable goals like increasing repetitions by 10 each week or reducing task completion time by specific percentages to track progress objectively and maintain motivation throughout the recovery journey.
Explore rehabilitation kits and aids for motor recovery
After understanding how motor recovery works and which exercises drive results, the next step involves accessing tools that make consistent practice achievable and engaging. Tisale Rehab specializes in rehabilitation kits designed specifically for stroke and cerebral palsy recovery, offering evidence-based solutions that work in both home and clinical settings. These products transform repetitive exercises into interactive experiences that maintain motivation during the intensive practice needed for neuroplastic changes.
The rehabilitation aids catalog includes options for every recovery stage and functional goal, from basic mobility support to advanced fine motor training. Whether you need hand therapy tools, balance equipment, or comprehensive therapy kits, these clinically proven devices help you maximize the critical early recovery window while supporting continued progress beyond the first year. Explore how the right rehabilitation equipment can complement your therapy program and accelerate your path toward greater independence.
Frequently asked questions
What is the typical timeline for motor recovery after stroke?
Motor recovery timelines vary widely based on stroke severity, location, and individual factors, but most significant improvement occurs within the first three to six months post-injury when the brain shows heightened neuroplasticity. This period represents a critical window for intensive rehabilitation that can dramatically impact long-term outcomes. However, continued recovery remains possible well beyond one year with consistent rehabilitation and ongoing neuroplastic changes, especially when patients maintain regular exercise practice. Early intervention and strong adherence to therapy protocols accelerate progress during both the acute recovery phase and extended rehabilitation period.
How can caregivers support motor recovery effectively?
Caregivers play a crucial role by encouraging consistent exercise participation and providing positive reinforcement that sustains motivation during challenging rehabilitation periods. Helping adapt the home environment to facilitate safe practice and mobility, such as installing grab bars or removing tripping hazards, enables more frequent independent practice. Regular communication with therapists ensures home exercises align with clinical goals and allows caregivers to reinforce proper technique. Creating a structured daily routine that includes dedicated exercise time helps establish consistency, while celebrating small victories maintains the patient’s emotional resilience throughout the recovery journey.
What role does motivation play in successful motor recovery?
Motivation is critical for sustaining the intensive and repetitive rehabilitation exercises required to drive neuroplastic brain changes and functional improvements. Without strong motivation, patients struggle to complete the hundreds of daily repetitions needed for meaningful recovery, leading to slower progress and potential plateaus. Techniques to boost motivation include setting specific, measurable goals, tracking progress visually with charts or apps, and using engaging rehabilitation tools that make practice enjoyable rather than tedious. Caregiver and therapist support enhances patient commitment by providing accountability, encouragement during setbacks, and recognition of achievements that might otherwise go unnoticed.
Recommended
38
Get inspired by a stroke survival story
It's a very good "gaming" therapy.
I had a stroke 9 years ago and have tried many different therapies. I really like the gaming aspect offered by MusicGlove. I have only been using this kit for a month and I can already see some progress. It helps me a lot to stay motivated. It's really amazing...
In summary, I really like MusicGlove. MusicGlove.
Tomasz S. (04.03.2020)



