How to create a therapy plan for a stroke patient step by step
Every neurological rehabilitation therapist in the UK knows the challenge of working with stroke patients, where a single template is never enough. Effective therapy planning requires not only knowledge of techniques but, above all, precise, individual functional diagnostics and consideration of the emotional and cognitive aspects of recovery. Go through the most important steps of building an effective therapy plan based on proven practices and current clinical knowledge.
- Step 1: Collect detailed patient data
- Step 2: Set individual therapeutic goals
- Step 3: Select appropriate rehabilitation methods and tools
- Step 4: Create a schedule and plan progress monitoring
- Step 5: Verify plan effectiveness and introduce corrections
Brief Summary
| Key Point | Explanation |
|---|---|
| 1. Collect comprehensive patient data | Accurate assessment of neurological status influences the further rehabilitation process and the setting of therapeutic goals. |
| 2. Set individual therapeutic goals | Goals should be realistic, measurable, and tailored to the patient's needs to increase their motivation. |
| 3. Select appropriate methods and tools | The choice of rehabilitation techniques must be related to the patient's individual deficits and therapeutic goals. |
| 4. Monitor progress and adapt the plan | Regular assessment of progress and ongoing adjustment of therapy methods are crucial for rehabilitation effectiveness. |
| 5. Communicate changes to the patient | It is important that the patient is kept informed about progress and any changes to the therapeutic plan. |
Step 1: Collect detailed patient data
Gathering comprehensive information about the patient is the foundation of the entire rehabilitation process. Before you propose specific exercises or therapeutic strategies, you must understand who you are really working with. This data collection phase will determine what every subsequent stage of treatment looks like and how effectively you will be able to achieve the set goals.
Start by looking at the patient's entire situation from a neurological and functional perspective. You need information about the mobility of their limbs, ability to maintain balance, state of cognitive functions, and speech ability. But that is just the beginning. Remember that assessing the patient's neurological status also includes their level of efficiency in activities of daily living and emotional state. These elements can have a huge impact on motivation for therapy and real progress in rehabilitation.
Collect data regarding the patient's health history before the stroke, their cognitive functions now, level of independence in performing daily tasks, and the social support they have access to. Talk to the patient and their family about their expectations, fears, and priorities. Does the patient wish to return to work? Do they want to be able to dress themselves? Is their main goal to improve hand or leg function? These details will shape the entire trajectory of therapy. An individual approach based on accurate functional diagnostics will allow you to create precise, measurable therapeutic goals tailored exactly to the given patient's situation.
Do not overlook the psychosocial aspect either. A stroke is not just a neurological issue; it is an event that changes the life of the entire family. Take a moment to understand the patient's emotional concerns, whether they have access to support from loved ones, or if they are struggling with depression or fear. This information will change the way you communicate with the patient and how you motivate them to act.
Pro Tip Create a standardised assessment form that you fill out systematically for every patient. This will save time, reduce the risk of missing important information, and make it easier to track progress over time.
Step 2: Set individual therapeutic goals
This is where the plan takes concrete shape. After collecting all the data about the patient, you must now transform this information into clear, measurable goals that will serve as a signpost for the entire therapy. Goal setting is not a one-time activity, but a process that requires thought and dialogue with the patient and their family.
Start with what is really important to your patient. Therapeutic goals must be tailored to the individual needs of the patient, not to general standards or what you consider important as a therapist. One patient dreams of returning to office work, another wants to play football with his son again, and a third simply wishes to dress independently and drink tea from a favourite mug. These differences are fundamental. Goals must be realistic and measurable, adapted to the patient's actual capabilities at the given moment, but at the same time ambitious enough to motivate them to act.
If the patient said their dream is to return to work, you cannot simply write "return to work" in the plan. That is too general. Instead, break this goal down into smaller, achievable stages. It might look like this: within four weeks, the patient should regain enough strength in the lower limb to walk 50 metres without assistance; in eight weeks, they walk independently; and in three months, they can work in the office for four hours a day. Do you see the difference? Such goals give you and the patient a clear picture of progress and allow you both to see concrete achievements.
Do not forget about goals that go beyond pure physical function. If the patient has struggled with depression after the stroke, a goal might include regular participation in group activities or returning to a hobby they previously enjoyed. If the patient has problems with cognitive functions, it might be improving memory or concentration ability. Remember that therapeutic goals should include restoring independence in daily activities and returning to professional and social activity, but above all, they must be understandable and important to the patient.
Set goals in cooperation with the patient and their family. During the conversation, ask open questions, listen carefully, and write down what they say. Then paraphrase what you heard to ensure you understood their expectations correctly. This is a simple technique, but hugely important for building trust and ensuring that you are all working towards the same goal. Also remember that goals may change during therapy. As the patient progresses, it is possible they will want to work on something else or their level of aspiration will change. This is natural and should be reflected in a dynamic approach to planning.
Pro Tip Write down every goal using the SMART method: Specific, Measurable, Achievable, Relevant, and Time-bound. For example, instead of "improving walking ability", write "the patient will walk 100 metres independently, without assistance, by the end of the 6th week of therapy". This gives a clear standard of success.
Step 3: Select appropriate rehabilitation methods and tools
Now comes the time to choose specific tools and techniques that will work towards the patient's goals. The selection of rehabilitation methods is not a random decision. It must be strictly linked to the assessment of the patient's condition that you performed at the beginning, and to the goals you established together. Every patient is different, and every stroke leaves a different mark, which is why the approach must be completely personalised.

Start by analysing what deficits the patient has and which of them are priorities for achieving their goals. If the patient cannot move their hand independently, there is no point in starting with walking training. Instead, you will focus on re-educating hand movement. Methods such as Bobath, PNF, or Brunnström are commonly used in post-stroke therapy and focus on normalising muscle tone, movement re-education, and neuromuscular stimulation. These techniques have solid scientific foundations and have been proven in practice for decades. When deciding on a specific method, ensure you understand its principles and feel comfortable applying it.
Alongside traditional physiotherapy methods, also consider other tools that can support therapy. Electrical stimulation can be helpful in patients with severe paralysis, occupational therapy enables work on activities of daily living in a practical context, and speech therapy is essential for patients with speech disorders. The choice of methods includes various physiotherapeutic techniques, occupational therapy, and psychological support, tailored to the patient's unique needs, including passive and active exercises, manual therapy, and balance training. Modern rehabilitation is a combination of different approaches, and you as a therapist must be like a museum curator, choosing from the available collection what will best serve the patient.
Here is a summary of popular post-stroke rehabilitation methods and their main applications:
| Rehabilitation Method | Key Applications | Main Advantages |
|---|---|---|
| Bobath | Normalisation of muscle tone | Safe at every stage of stroke |
| PNF | Improvement of movement control and coordination | Flexibility to adapt to the patient |
| Brunnström | Phases of limb movement recovery | Clear plan of therapy stages |
| Occupational Therapy | Training of activities of daily living | Strengthens independence and motivation |
| Electrical Stimulation | Muscle support in severe paresis | Enables activation even in deep paralysis |
| Speech Therapy | Work on speech and communication | Also includes therapy of cognitive functions |
Do not forget about assistive tools. In times when access to modern rehabilitation technologies is becoming easier, it is worth considering the use of devices supporting the therapy process. These can be systems for motor training, tools supporting balance training, or mobile apps supporting cognitive functions. These tools can be particularly valuable during home exercises, where the patient works without therapist supervision. Remember, however, that a tool is just a tool. Your role as a therapist is to guide the process, adjust intensity, and monitor progress.
It is also important to prepare for changes. As the patient progresses, you will have to modify the methods used. What was appropriate in the third week of therapy might be too easy in the eighth week. Regular adaptation of therapeutic tools and methods is crucial for maintaining patient motivation and ensuring continuous progress. A review and potential change of approach should be conducted at least once every two weeks, depending on the pace of the patient's progress.
Pro Tip Create your own knowledge base of available methods and tools. Regularly read scientific publications regarding neurorehabilitation and participate in training to stay up to date with the latest solutions and techniques in the field.
Step 4: Create a schedule and plan progress monitoring
You already have the patient data, you have set the goals, and selected the methods. Now you must build a structure that will make everything work in a coordinated way. The therapy schedule is the skeleton of your plan, and progress monitoring is its brain. One without the other is simply chaos.
Starting to create a schedule requires making several concrete decisions. How often should the patient come for sessions? Will it be three times a week, or perhaps two? How long should each session be? The answers depend on the patient's condition, their goals, and the resources available in your clinic. Typically, in the initial phases of post-stroke rehabilitation, patients need more frequent sessions, and as they improve, they can move to less intensive exercises. The therapy schedule should be precisely planned, including regular rehabilitation sessions and periodic assessments of the patient's progress, to ensure systematic evaluation of motor, cognitive, and emotional functions. This is not just a matter of logistics, but also the psychological side of the process. The patient needs to know what they can count on and when they will see you.
Within the schedule, also plan home exercises. This is very important because sessions in the office are just the tip of the iceberg. The patient spends most of their time at home, and their progress also depends on how conscientiously they perform exercises between sessions. Describe exactly what exercises they should do, how often, and for how long. It is better to have three well-performed exercises daily than fourteen exercises performed poorly. Also consider whether rehabilitation at home will be supported by caregivers or if the patient will work independently.
Monitoring progress is a continuous process, not a one-time activity. Planning the schedule requires establishing the frequency and intensity of exercises and regular monitoring of progress through observation and functional tests. During every session, you should observe the patient and note your observations. Is the movement more fluid than last time? Does the patient feel less tired? Is their mood improving? In addition to clinical observation, also use formal functional tests. These can be simple things, like measuring the range of motion in a joint or the time in which the patient can rise from a chair. Such tests give you objective data that you can use.
Implement a documentation system that will reflect the patient's progress. This can be a traditional notebook or a more advanced electronic system. It is important to document not only clinical data but also information about how the patient feels, what fears they have, and how this affects their motivation. Conduct a formal progress review every two weeks. Compare the patient's current state with their previous measurements. Is the patient getting closer to their goals? Are you still on the right path, or do you need to change the approach?
It is also important to communicate with the patient about their progress. People tend to get frustrated when they don't see immediate results. Show them concrete data. Two weeks ago they couldn't walk 30 metres without assistance, now they walk 50 metres. This is an achievement. Such small victories build motivation and show the patient that their effort makes sense.
Below is an example schedule for monitoring rehabilitation progress:
| Assessment Frequency | Scope of Monitored Progress | Recommended Tools |
|---|---|---|
| Every session | Changes in mobility, well-being | Observation, interview |
| Every 2 weeks | Comparison of functional test results | Standard tests |
| Every month | Review of therapeutic goal achievement | Assessment form |
| After every change | Reaction to new method or intensity | Progress log |
Pro Tip Use simple assessment forms that you fill out consistently at every session. They contain standard questions and measurements that facilitate comparison of progress over time and reduce the risk of missing important changes in the patient's condition.
Step 5: Verify plan effectiveness and introduce corrections
The plan you created is not a document set in stone. It is a living, breathing guide that must react to what is happening with the patient in reality. Verifying effectiveness is the moment when you check if theory has met practice, and if you need to change anything.
Start by clearly defining what "lack of progress" means to you. It's not about the patient not becoming perfect in two weeks. It's about seeing no changes towards the set goals. If the patient was supposed to achieve a range of motion of 80 degrees in the ankle joint within four weeks, and in that time achieved only 65 degrees, that might be a signal that something needs to change. The effectiveness of a therapy plan requires regular assessment, which includes both monitoring progress in motor functions as well as psychological and social aspects. Do not focus only on measurable results. Also observe how the patient feels. Are they more motivated? Do they have less pain? Is their mood improving? These factors can be just as important as numbers.
When you identify an area where progress is slower than expected, instead of panic or frustration, consider the causes. Maybe the patient is not performing home exercises as conscientiously as they promised? Maybe the therapeutic method you chose is not optimal for this specific patient? Maybe the patient struggled with additional stress or a change in health status? The answers are usually in the conversation. Talk honestly with the patient. Find out what is happening between sessions, what their fears are, and what could help them motivate themselves better.
Verifying the effectiveness of the therapy plan requires continuous monitoring and documenting of the patient's progress, and when expected results are not seen, you modify the plan. This may mean changing therapeutic methods. If the patient does not respond well to the Bobath method, you can try PNF or another approach. It may also mean changing the intensity of exercises. Sometimes patients need more intensive training, and sometimes the opposite. It may also mean changing goals. If it turns out that the patient has more limited capabilities than you predicted, instead of sticking to impossible-to-achieve goals, it is better to change them to more realistic ones. This is not a failure. It is adapting to reality.
Also remember that sometimes a lack of visible progress may result from other causes. The patient might have had another stroke, an infection, or another medical event that interrupted rehabilitation. In such cases, the plan must be completely analysed and likely postponed. Flexibility is key.
Also communicate the way changes are communicated to the patient. You don't want them to feel like a failure if you change the plan. Instead, explain to them that you are observing their progress, you see where they have difficulties, and you want to adjust strategies to be more effective. Such an approach builds trust and shows the patient that you are truly taking care of them.
Pro Tip Conduct a full assessment of plan effectiveness every four to six weeks. During this time, perform all the standard tests you did at the beginning and compare the results. This will give you objective data that can justify introducing changes to the therapy plan.
An effective therapy plan is the key to success in stroke rehabilitation
Creating an individual therapy plan requires precise assessment, setting realistic goals, and selecting appropriate rehabilitation methods. This process often encounters challenges such as selecting tools, patient motivation, or monitoring effects. Thanks to innovative solutions available at UdarRehab / TiSale LTD, you can effectively enrich your therapy plan with advanced devices tailored to the patient's unique needs.
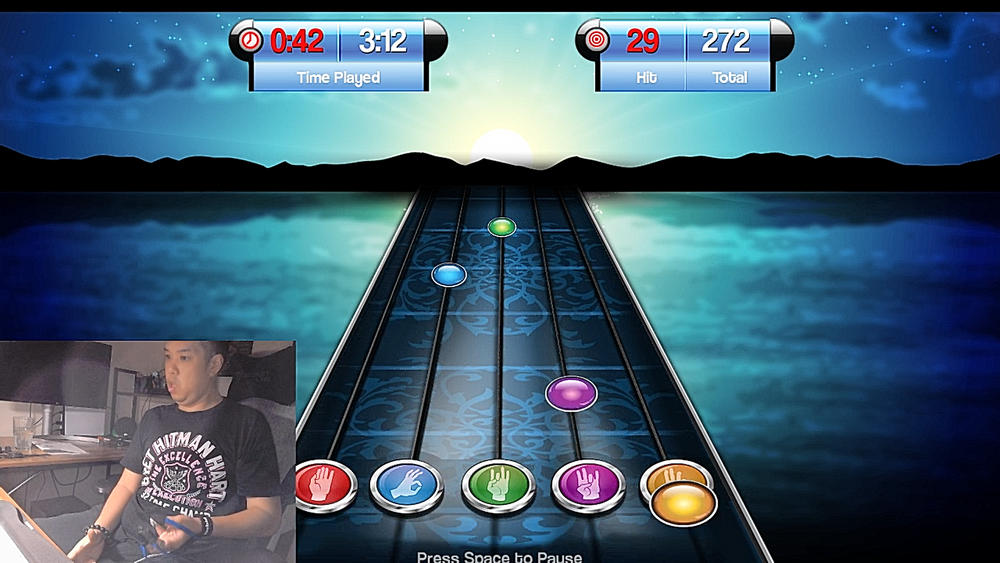
Start rehabilitating with us, using modern methods and medical equipment that improve therapy effectiveness and realistically support the return to independence. Visit Rehabilitate with us to learn about available solutions and see how equipment like FitMi or MusicGlove can change the course of your rehabilitation. Do not delay – the best moment to act is now at https://tisalerehab.com!
Frequently Asked Questions
What data should I collect about a stroke patient before starting therapy?
Collect detailed information regarding limb mobility, balance, and the state of the patient's cognitive and emotional functions. Also determine their level of independence in daily activities and the social support available to them.
How to set therapeutic goals for a stroke patient?
Therapeutic goals should be tailored to the individual needs of the patient and fully stem from their priorities. Set SMART goals that are specific, measurable, achievable, relevant, and time-bound, for example, "the patient will regain the ability to dress independently within three months".
What rehabilitation methods are appropriate for a stroke patient?
Select rehabilitation methods based on the patient's individual needs and the data gathered about them. Methods such as Bobath, PNF, or occupational therapy are popular and effective, and the selection should be related to the patient's current motor limitations.
How often should I monitor the patient's progress during therapy?
Patient progress should be monitored during every rehabilitation session and every two weeks using formal functional tests. Document changes and achievements to adjust the therapy plan to the patient's actual needs.
What to do if I don't see progress in a stroke patient?
Analyse the reasons for the lack of progress by talking to the patient about their experiences and difficulties. Modify the therapy plan by changing methods, exercise intensity, or improving communication to better motivate the patient.
How to create a therapy schedule for a stroke patient?
Plan the schedule taking into account the frequency of sessions and the duration of each to enable effective rehabilitation. For example, establish that the patient will participate in sessions three times a week for an hour each, and define home exercises they will perform between sessions.
Recommendations
38
Zainspiruj się historią powrotu do zdrowia po udarze mózgu
Moja opinia o MusicGlove
Oto moja krótka opinia - recenzja MusicGlove. 3 października 2020 r. przeszedłem udar krwotoczny mózgu. Kupiłem MusicGlove po około 4 miesiącach hospitalizacji. Mogłem wtedy poruszać palcami, ale - delikatnie mówiąc - "niezbyt" skutecznie. Prawdę mówiąc, nie potrafiłem chwytać małych przedmiotów, takich jak długopis czy drobne rzeczy, i pisałem tylko zdrową ręką. Dwa miesiące użytkowania. Potrafię już trochę pisać - krótko, bo krótko - ale mogę już napisać coś moją niesprawną ręką, co mnie uspokaja i daje nadzieję na powrót do pracy. Nie stanie się to od razu, jednak ta myśl popycha mnie do przodu i mam teraz jasny i realistyczny cel. Jedynym minusem jest może ograniczona liczba piosenek. Więc muzyka czasami się powtarza. Aha!... Upewnijcie się, że macie odpowiednią rękawicę - właściwy rozmiar - nie może być ani za duża, ani za mała! Zamówiłem rozmiar, który okazał się za duży, ale obsługa klienta była doskonała i szybka, sprawnie i szybko wymienili mi rozmiar. Zestaw jest łatwy w instalacji, dosłownie "podłącz i używaj". Podsumowując: Brawo dla mnie i Brawo dla TiSale Rehab.
Nikodem (24.02.2021)